INTRODUCTION
Endoscopic submucosal dissection (ESD) is widely used as a treatment for gastric cancers that are associated with a low risk of nodal metastasis. However, the prevalence of postoperative bleeding, a complication of ESD, is approximately 0%ā15.6% and it reduces a patientās quality of life [1,2]. The number of patients receiving antithrombotic agents is expected to increase in the future as the populations age; therefore, there is a concern that the incidence of post-ESD bleeding will also grow [3]. However, no effective hemostatic methods for preventing such bleeding have been established yet.
Recently, the use of fibrin glue to attach polyglycolic acid (PGA) sheets (NeoveilĀ® 0.15-mm sheets; Gunze Ltd., Osaka, Japan) to ulcer beds following ESD has been reported as a promising method in preventing post-ESD bleeding [4-8]. Although this method has already been demonstrated to be useful in many surgical fields [9-12], it is difficult to use it to treat post-ESD ulcers in the gastrointestinal tract, especially, when the sheets have to be applied against gravity. Takimoto et al. reported a method for covering post-ESD ulcers with PGA sheets [13]. However, it requires a long time because the PGA sheets become wet and massive when they are passed one-by-one through a forceps channel. Additionally, Takegawa et al. reported that when PGA sheets are delivered and fixed to the stomach they become wet with saliva or mucus, which degrades their adhesive power [14]. To address these issues, Takao et al. developed an envelope-based system for delivering PGA sheets to the stomach (the envelope method) in 2017 [15]. In this method, PGA sheets are stored in an envelope during their transport, which allows them to be transported and fixed to the stomach rapidly without exposing them to saliva or mucus (Fig. 1A) [15]. Their study revealed that PGA sheets can be efficiently delivered and fixed to the digestive tract. However, this method was only demonstrated to be effective for treating ulcers in resected stomachs when the sheets were applied in the direction of gravity (such ulcers are referred to as gravitational ulcers hereafter); the delivery and fixation of PGA sheets is easy in such ulcers.
It remains unclear whether the envelope method is useful for treating ulcers in the living body and against the direction of gravity (such ulcers are referred to as anti-gravitational ulcers hereafter). This study was performed to demonstrate the usefulness of the envelope method for treating both gravitational and anti-gravitational post-ESD ulcers in living porcine stomachs.
MATERIALS AND METHODS
This study was approved by KM Biologics institutional animal care and use committee (approval number: B18-024) and was conducted in compliance with the relevant regulations regarding humane treatment of laboratory animals.
The time required to deliver PGA sheets into the stomach of a living pig and fix them in place with or against gravity as part of the treatment of post-ESD ulcers (PGA sheet application time) was compared between the conventional and envelope methods. Additionally, after PGA sheets were fixed in place in the anti-gravitational or gravitational direction with fibrin glue (Bolheal; KM Biologics Co., Ltd., Kumamoto, Japan) using the conventional or envelope method, endoscopic and histological examinations were performed and the results were compared between the methods.
Artificial ulcer creation
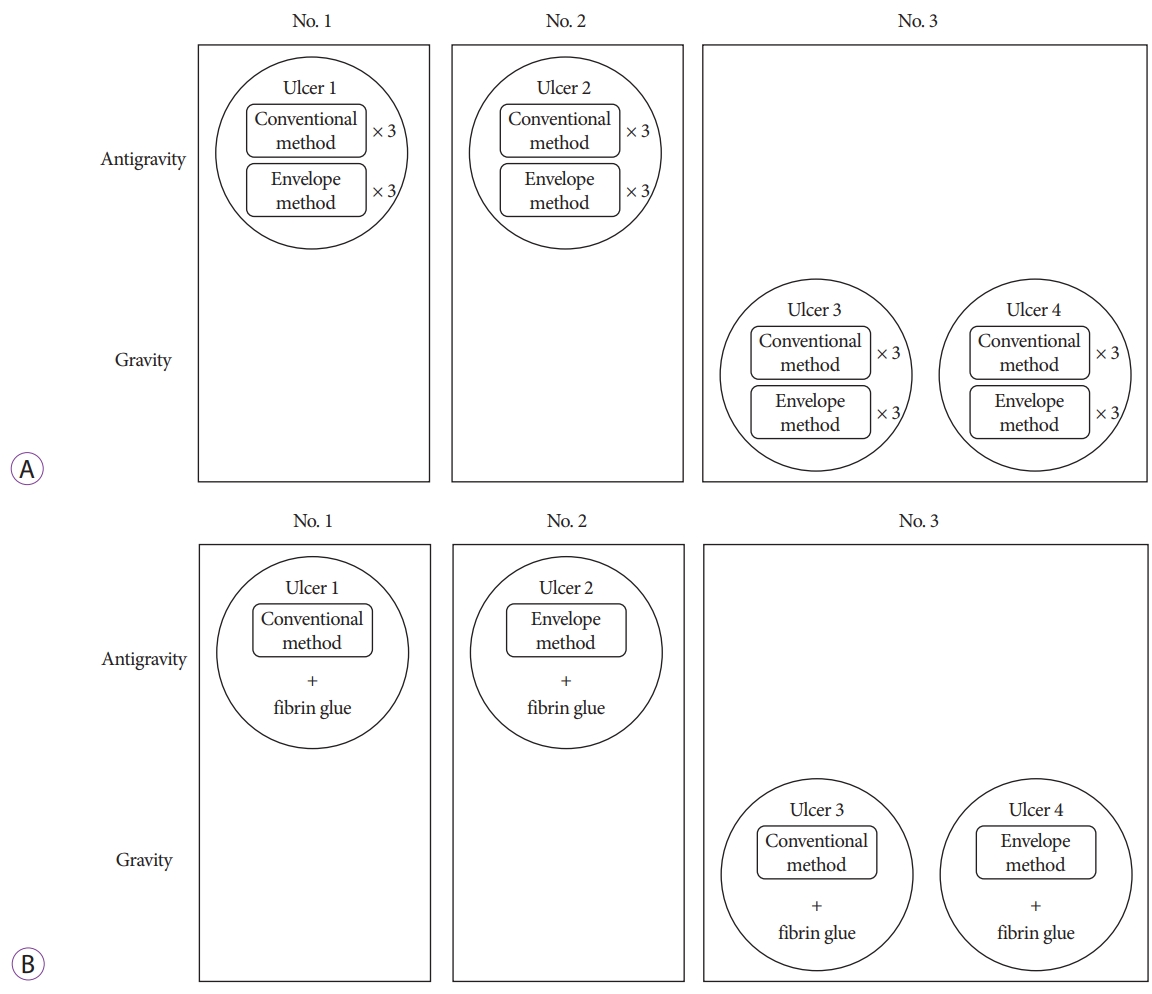
Three male pigs (Large White X Landrace or Large White, age: 2ā3 months, body weight: 20ā30 kg) were used for this study. Tracheal intubation was performed under general anesthesia. An upper gastrointestinal endoscope (GIF-H260; Olympus Co., Tokyo, Japan) was inserted through an overtube (TOP overtube 17, double type; Top Co., Ltd., Tokyo, Japan) into the stomach. Fig. 2. depicts the methods by which PGA sheets were used to cover the ulcers and fixed in place with fibrin glue.
In two living pigs (animals 1 and 2), two anti-gravitational post-ESD ulcers (ulcers 1 and 2) were created in the stomach. Additionally, two gravitational post-ESD ulcers (ulcers 3 and 4) were created in the stomach of another living pig (animal 3) (Fig. 2A). To delineate each ulcer site, a circular piece of paper was placed on the mucosa, and marks were made around the paper to ensure that the ulcer size was constant. Glyceol (Glyceol injection 20 g/200 mL; Chugai Pharmaceutical Co., Ltd., Tokyo, Japan) was locally injected into the marked regions. An electric knife (Flush knife BTĀ®, DK2618JB; Fujifilm Co., Tokyo, Japan or IT knife 2Ā®, KD-611L; Olympus) and an electric generator (ESG-400; Olympus) were used for the ESD. After the ESD was completed, the blood vessels in the ulcer floor were coagulated using hemostatic forceps (CoagrasperĀ®, FD-411QR; Olympus).
Polyglycolic acid sheet delivery and fixation
In the conventional method, 15Ć7-mm PGA sheets were grasped with biopsy forceps, transported to the stomach oneby-one through a forceps channel, and attached to the ulcer floor, as reported by Takimoto et al. [13]. The forceps used in the conventional method were the same as those used by Takao et al. in 2017 (FB-25K-1; Olympus), which are considered to be less likely to become tangled up in the fibers of the PGA sheets than other types of forceps (Supplementary Video 1) [15].
In the envelope method, large or medium-sized PGA sheets, which had been cut to match the size of the target ulcer, and 15Ć7-mm PGA sheets were placed in a two-layered container envelope (BolhealĀ® GI envelope; Nipro Co., Osaka, Japan) (Fig. 1B). Before the endoscope was inserted, the radio-opaque string (Fig. 1A; white arrow) attached to the envelope, which protruded from the tip of the endoscope was grasped using the hemostatic forceps. The envelope body was held with the fingers so that the transparent film was in contact with the endoscope. Lubricating jelly was applied to the absorbent surface of the envelope. The endoscope was inserted through a mouthpiece, and the envelope was passed into the stomach. It was placed on the gravitational side of the stomach so that its absorbent surface adhered tightly to the mucosa. A largeor medium-sized sheet was removed from the envelope using the hemostatic forceps and fixed to the ulcer floor. When an ulcer could not be fully covered using a large sheet, additional small sheets were taken from the envelope and attached to the ulcer site. As the PGA sheets stored in the envelope were less likely to become wet and fold, we were able to use hemostatic forceps. Therefore, it was not necessary to change forceps after the post-ESD hemostatic coagulation procedure (Supplementary Video 2).
The two post-ESD ulcers on the gravitational side and the two post-ESD ulcers on the anti-gravitational side were covered repeatedly (three times for each ulcer) with PGA sheets using the conventional or envelope method. Therefore, the time required for the delivery and fixation of the PGA sheets (PGA sheet application time) was measured six times for each method, as depicted in Fig. 2A. To standardize the site and size of ulcers between the two methods, after a PGA sheet had been stuck in place using one method, it was completely removed using the forceps. Subsequently, the other method was used to paste the sheet against the same ulcer. In order to reduce the differences between the application time and condition of the ulcer floor between the conventional method and envelope method due to edema caused by PGA sheet application and detachment, the order of the conventional method and envelope method was changed for each procedure.
Measurements
PGA sheet application time was defined as the time required to transport the PGA sheets into the stomach and cover the entire ulcer floor. The measurement of the PGA sheet application time started when the tip of the endoscope was placed near the ulcer and the forceps holding the PGA sheet were inserted into the forceps channel in the conventional method, and when the endoscope and envelope passed through the mouthpiece in the envelope method. As it is difficult to create ulcers of the same size and the size of the ulcer changes depending on the volume of air in the stomach, the diameter of each ulcer was measured using a scale (M1-2U; Olympus) before each application procedure, and the application time per unit area was compared. All procedures were performed by a single operator to minimize interoperator differences in the delivery or fixation of the PGA sheets. As the operator was familiar with both methods in advance, any effects of the learning curve were small, but both methods were used alternately to reduce the learning curve effects to the greatest degree possible.
Histological evaluation
PGA sheets were attached using the conventional or envelope method to anti-gravitational (ulcers 1 and 2) or gravitational (ulcers 3 and 4) ulcers. They were then fixed in place with fibrin glue (Fig. 2B). The fibrin glue was applied using a double-lumen catheter (BolhealĀ® double-lumen catheter; Nipro), which was specifically developed for use during the application of BolhealĀ®. The catheter tip was then used to press the PGA sheet on the ulcer (the force used was not sufficient to displace the PGA sheet) so that solution A permeated the entire sheet. Subsequently, solution B was applied to the ulcer floor similarly. After the sheets were fixed in place, the pigs were immediately euthanized. After the ulcers had been fixed in 10% neutral buffered formalin, paraffin sections were prepared in the standard manner, stained with hematoxylin and eosin, and evaluated histologically.
Statistics
MannāWhitneyās U test was used to detect significant differences in the PGA sheet application time. The minimum number of ulcers required was calculated to be six. Results associated with two-tailed p-values <0.05 were considered to be significant. The effect size was computed based on previous results [15]. All statistical analyses were conducted using the EZR software (Saitama Medical Center, Jichi Medical University, Saitama, Japan) [16].
RESULTS
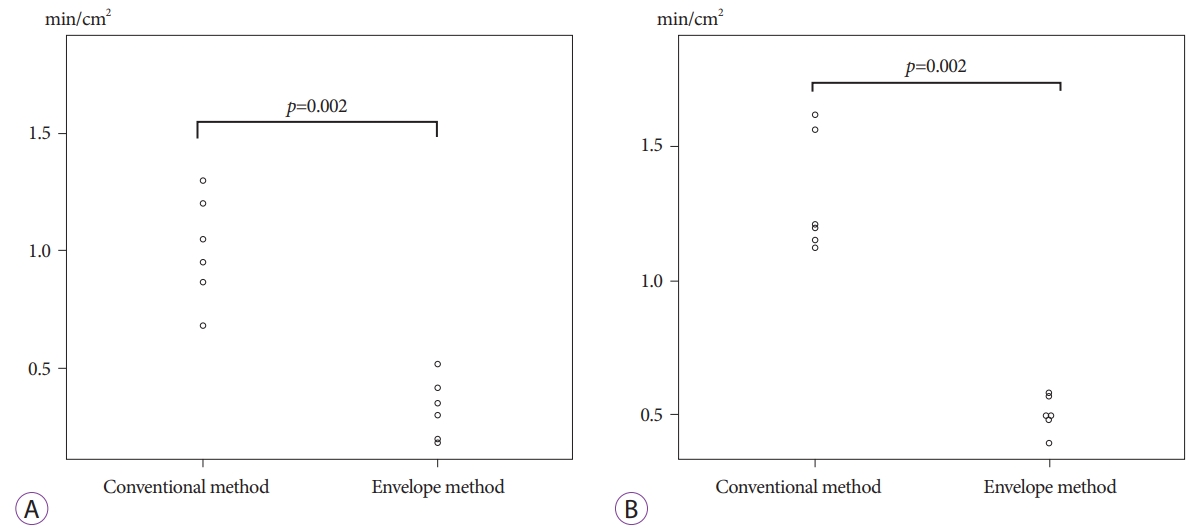
PGA sheet application times for the gravitational ulcers are summarized in Table 1 and Fig. 3A. The application times for the anti-gravitational ulcers are summarized in Table 2 and Fig. 3B.
The median (range) PGA sheet application time per unit area for the gravitational ulcers was 1.00 (0.68ā1.30) min/cm2 and 0.32 (0.18ā0.52) min/cm2 in the conventional and envelope approach, respectively. The median PGA sheet application time per unit area in the envelope group for the gravitational ulcers was significantly shorter than that in the conventional group (p=0.002). The median (range) PGA sheet application time per unit area for the anti-gravitational ulcers was 1.20 (1.13ā1.63) min/cm2 and 0.50 (0.39ā0.58) min/cm2 in the conventional and envelope approach, respectively. The median PGA sheet application time per unit area in the envelope group for the anti-gravitational ulcers was significantly shorter than that in the conventional group (p=0.002). There was no significant difference in the application time in each group depending on the order of the procedures. Additionally, the application time per unit area in the envelope method was shorter than that in the conventional method in each procedure.
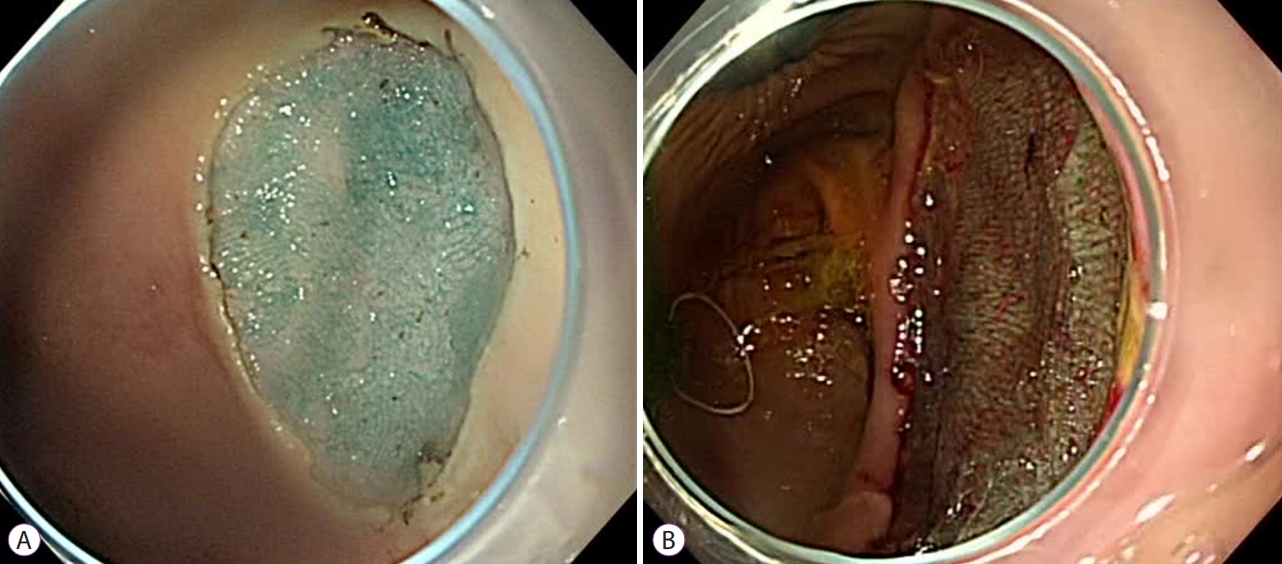
In the endoscopic examinations of the anti-gravitational ulcer sites, the ulcer floor revealed uneven PGA sheets in the conventional group and some PGA sheets had clumped together (Fig. 4A), whereas the endoscopic examinations of the anti-gravitational ulcer sites revealed appropriately applied PGA sheets in the envelope groupāthe sheets were flat and only slight overlapping of the sheets was seen in all six procedures (Fig. 4B).
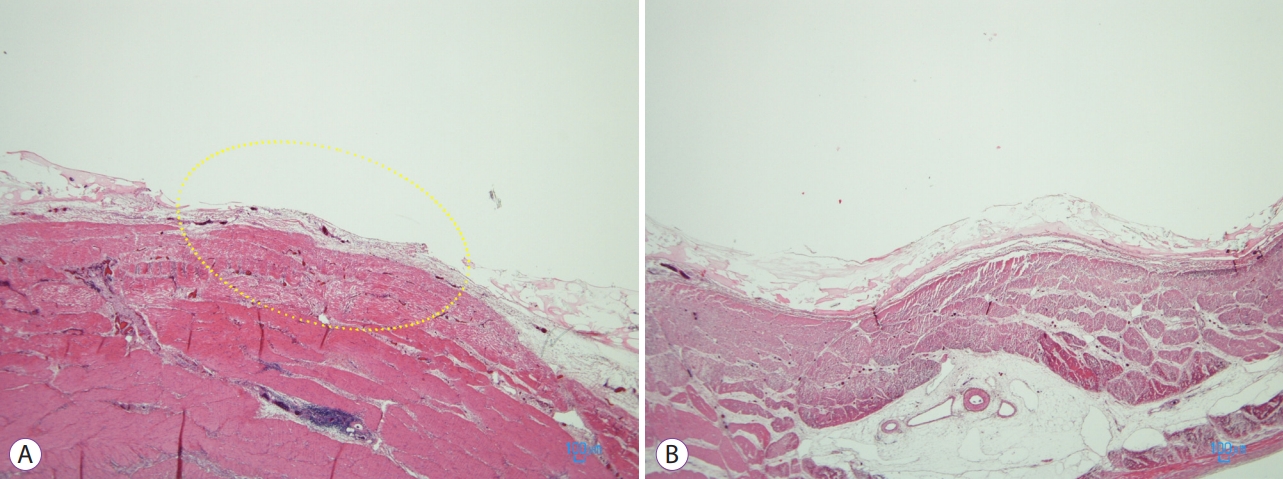
Histological examinations of the anti-gravitational ulcer treated using the conventional method revealed that the ulcer floor was partly uncovered because there were gaps between the PGA sheets (Fig. 5A). On the other hand, histological examinations of the anti-gravitational ulcers treated using the envelope method demonstrated that the ulcer floor was uniformly covered with a mixture of PGA sheets and fibrin glue (Fig. 5B). In the anti-gravitational ulcers treated using the envelope method, the thickness of one layer of PGA sheets/fibrin glue was approximately 300 Ī¼m.
DISCUSSION
In this study, three important findings were observed in in vivo experiments. First, the PGA sheets were transported and fixed to the anti-gravitational ulcers significantly more quickly in the envelope group than they were in the conventional group. Second, in the envelope group, endoscopic examinations revealed that the sheets were fixed to the anti-gravitational ulcers appropriately, i.e., they laid flat across the ulcer sites without gaps between the sheets. Third, histological examinations confirmed that the sheets were fixed in the anti-gravitational ulcers appropriately in the envelope group.
As mentioned above, PGA sheets were transported and fixed to the gravitational ulcers significantly more quickly in the envelope group than that in the conventional group. In clinical practice, PGA sheets are often fixed to ulcers using the conventional method after ESD [13,17,18]. However, as indicated above, it takes longer time to apply the sheets in the conventional method because they get wet. Particularly, fixing PGA sheets to the anti-gravitational ulcer sites was more difficult using the conventional method because the sheets that had formed a wet mass in the forceps channel tended to drop downwards due to their weight. In the envelope group, several PGA sheets, including large sheets, were transported into the stomach in a dry state. Therefore, it was possible to quickly fix them in place, even in anti-gravitational ulcers, which was difficult in the past.
Regarding our second finding, in the envelope group, endoscopic examinations demonstrated that the sheets were appropriately fixed on the anti-gravitational ulcer sites under dry conditions, i.e., when the sheets were not exposed to saliva or mucus in vivo. A previous study demonstrated that when exposed to saliva or mucus, fibrin glue does not permeate PGA sheets, thereby, reducing their adherence to the ulcer floor [14]. In 2015, Takao et al. transported PGA sheets packaged in folded films into the gastrointestinal tract in living pigs [19]. However, in some cases the PGA sheets became moist during their transportation [19]. In contrast, in the envelope group in the present study, all of the transported sheets were delivered without becoming wet, thus, indicating that the envelope method is more effective than the conventional method at protecting PGA sheets from saliva and mucus. The current study demonstrated that PGA sheets can be delivered to the stomach in a dry state, even in vivo.
As for our third finding, in the envelope group, histological examinations demonstrated that PGA sheets were appropriately fixed to the anti-gravitational ulcer sites. As the sheets were light when they were dry, large sheets could be fixed appropriately to the ulcer sites without any wrinkles. When fibrin glue is spread on anti-gravitational ulcer floors, one concern is that it might be difficult to ensure that a sufficient amount of fibrin glue remains on the ulcer floor because of the effects of gravity on the liquid glue. In the present study, the PGA sheet/fibrin glue layers covering the anti-gravitational ulcer treated using the envelope method were 300-Ī¼m thick. The PGA sheets used in this study were only 150-Ī¼m thick. Therefore, it was demonstrated that a sufficient amount of the fibrin glue was retained.
Since 2012, when Takimoto et al. reported a method for applying PGA sheets to duodenal ESD ulcers using fibrin glue, several proposals have been made regarding the delivery of PGA sheets to the gastrointestinal tract [13,15,18,20-22]. Of those methods, the only device delivery station system (DDSS) except for the envelope method may be capable of delivering and pasting PGA sheets into the stomach without exposure to saliva or gastric juice. However, it was reported that some ring-shaped threads need to be tied to the PGA sheet before using the DDSS delivery system. The DDSS must be clipped onto the gastric mucosa before removing the PGA sheets from it. In contrast, we can easily remove the PGA sheet from the envelope without such accessories as the thread on the PGA sheet. Furthermore, we do not have to clip the envelope on the gastric mucosa because the envelope tends to become more adhesive to the mucosa due to the water-absorbing material on the back surface of the envelope. We believe that the envelope method is more useful and secure delivery system to allow PGA sheets to be applied to post-ESD ulcer without exposure of saliva or mucus.
We must ultimately demonstrate whether the application of PGA sheets can prevent the complications of post-ESD bleeding and perforation. However, in order to verify whether PGA sheets are useful in preventing these complications, it is a precondition that the PGA sheets can be delivered to the ESD site efficiently and attached securely on the ulcer floor in vivo. We demonstrated that the envelope method allows PGA sheets to be applied to post-ESD ulcers not only with gravity but also against gravity faster and more securely than the conventional method in living pigs.
Future prospects
The recent increases in the number of patients taking oral antithrombotic drugs and the number of endoscopic procedures in patients who are on antithrombotic drugs have raised concerns about the frequency of bleeding after endoscopic treatment. The envelope we used in this study has completed the pharmaceutical approval process and is now entering the preparatory stages of commercialization. The envelope method should be examined in a clinical trial to determine whether reliable transportation can be achieved irrespective of the location of the ulcer. Ultimately, a trial will be needed to demonstrate whether shielding with PGA sheets can prevent complications, such as postoperative bleeding and delayed perforation after ESD.
Limitations
The examinations were conducted by a single operator who was skilled in the procedure. Additionally, the structures of porcine and human stomachs differ slightly. Future clinical trials involving multiple endoscopists should be conducted at multiple facilities.
The envelope method can be used to rapidly transport PGA sheets into living porcine stomachs and fix them in place appropriately. This method can be used to treat both gravitational and anti-gravitational ulcers.