INTRODUCTION
Localized lymphoid hyperplasia of the large intestine is rare and appears exclusively in the rectum [1,2]. This lesion is also known as lymphoid polyp, benign lymphoid polyp, and rectal tonsil [3,4]. Although an association with infections such as chlamydia or EpsteinŌĆōBarr virus has been reported [5,6], its etiology remains unknown. Since rectal tonsils are benign, we recommend it should be differentiated from other lymphomas such as carcinoids or the polypoid type of mucosa-associated lymphoid tissue (MALT) lymphomas due to its similarity to these tumors upon gross examination [1,7,8]. In this report, we describe a case of twin rectal tonsils that was diagnosed by immunohistochemistry following endoscopic mucosal resection.
CASE REPORT
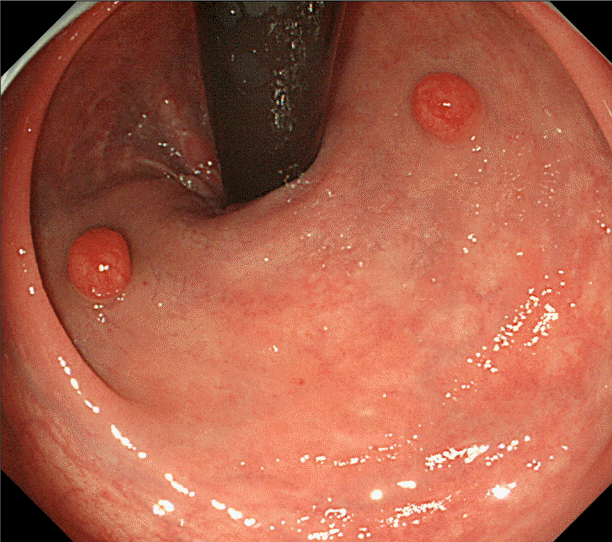
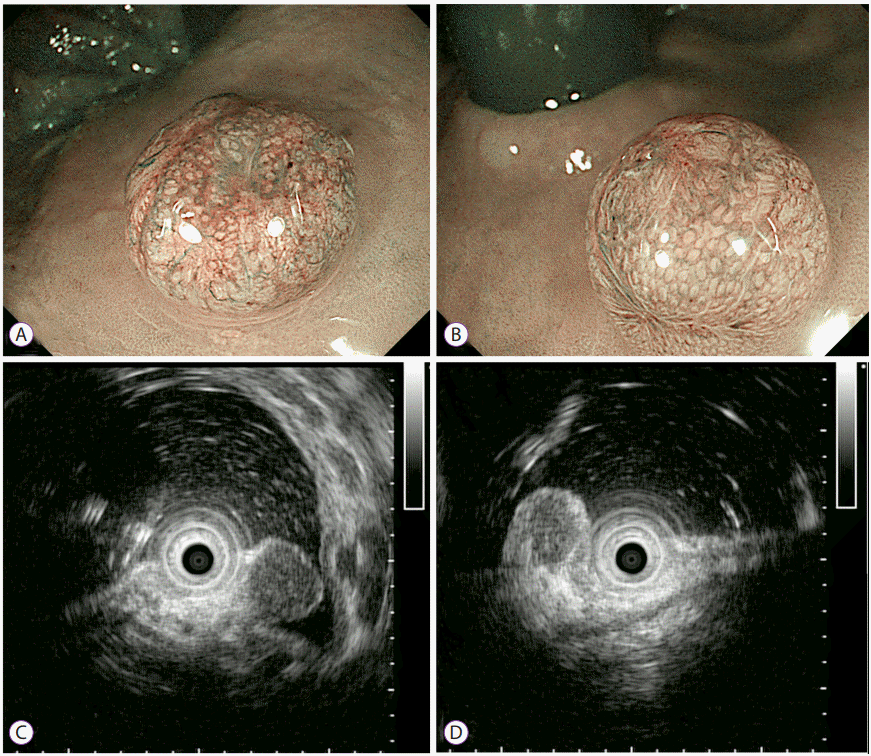
A 41-year-old man with a long history of psoriasis, and was taking 150 mg of oral cyclosporine daily and using a topical steroid medication, underwent a computed tomography (CT) scan as a systemic screening for the administration of anti-tumor necrosis factor (TNF)-alpha antibodies. He was referred to our department for further evaluation after an increased density of mesenteric adipose tissue was revealed in his abdomen. His past medical history was unremarkable except the skin disease, and laboratory data showed no other abnormalities. Colonoscopy in retroflexed view revealed two 5-mm-sized nodules that were identical in appearance and were located opposite of each other on the left and right sides of the lower rectum (Fig. 1). These nodules were both slightly red in color, and observations by narrow-band imaging (NBI) with magnification revealed dilated branches of vessels on the mucosal surface (Fig. 2A, B). Endoscopic ultrasound (EUS) revealed well-demarcated small hypoechoic areas in the lamina propria (Fig. 2C, D). We performed a biopsy but were unable to make a definitive final diagnosis due to the small tissue samples. Therefore, an endoscopic mucosal resection was conducted in order to make a more precise diagnosis and to remove the nodules. Histopathologically, both lesions were mainly located in the submucosa and consisted of prominent lymphoid follicles with germinal centers of various sizes (Fig. 3A). The polarization of the follicle and the presence of tingible body macrophages suggested a reactive rather than neoplastic follicular process. No immunoreactivity with Bcl-2 was observed in the germinal centers (Fig. 3B). Aggregates of CD20-positive lymphoid cells were distributed in the mucosa. Although small numbers of B cells were seen in the glands, epithelial destruction was not observed. Immunohistochemical staining for kappa and lambda light chains revealed a polyclonal pattern (Fig. 3C, D). Therefore, these lesions were diagnosed as rectal tonsils with no malignancy.
DISCUSSION
Since 2005, 21 cases of rectal tonsil, including ours, have been reported in the scientific literature [1,2,5,7-10] (Table 1). These cases comprised 8 males and 13 females aged 1ŌĆō71 years. Four of the 21 cases presented with multiple lesions. Although the endoscopic appearance of rectal tonsils varies among types such as polypoid (38%), sessile (33%), and nodule or mass (29%), most rectal tonsils appear to be covered with a normal epithelium and present as submucosal lesions. While their conventional endoscopic and endosonographic appearance are somewhat similar to those of the rectal tonsil, carcinoid tumors more commonly appear as yellow-colored solitary lesions. These characteristics could be used as distinguishing features for diagnosing rectal tonsils. Although the nodules in our case demonstrated dilated branches of vessels on the mucosal surface under NBI with magnification, it remains unclear whether this finding is a characteristic of rectal tonsils. Additionally, in our case, there was a discrepancy in the location of the rectal tonsil as observed with EUS and histopathology. This may have been due to the shape of the lesion since a significant portion of it was protruding into the lamina propria. Therefore, accumulation of the rectal tonsil is needed for it to be observed under NBI with magnification and EUS.
Previous studies have also reported rectal tonsils that mimic lymphomas and MALT lymphomas [1,9]. These lesions were diagnosed as rectal tonsils by endoscopic removal followed by immunohistochemistry. Histologically, rectal tonsils are characterized by large lymphoid follicles accompanied with active germinal centers in the submucosa. No colonized lymphoid follicles or lymphoepithelial lesions (LELs) have been reported in rectal tonsils. The diagnosis of MALT lymphomas is usually based on histopathological morphology such as a prominent marginal zone and the presence of LELs. Immunohistochemical monoclonality including CD43 and/or the presence of immunoglobulin light chain restrictions are also characteristics of MALT [1]. Our present case demonstrated polyclonal reactivity for kappa and lambda light chains and a lack of Bcl-2 staining in the follicles. Based on these findings, MALT and follicular lymphoma were excluded in the diagnosis.
In conclusion, rectal tonsils are a benign reactive change, although it is similar in endoscopic appearance to carcinoids, MALTs, or follicular lymphomas. In a superficial or small biopsy, rectal tonsils can be incorrectly diagnosed as malignant lymphomas. For an appropriate diagnosis and treatment of rectal tonsils, complete resection by endoscopy, histopathological examination, and immunohistochemical evaluations are recommended [1,5].