How Do I Overcome Difficulties in Insertion?
Article information
Abstract
Demand for colonoscopy is increasing because it is an important tool not only for screening of colorectal neoplasm but also for resection of such lesions in early stage. Cecal intubation requires expertise on shortening of the examination time and improvement of the cecal intubation rate without causing pain to the patients. About 5% to 10% of patients still experience difficulties or failure of the cecal intubation. There are number of factors that affect the difficulty of the colonoscopy such as technical skill of the endoscopist, angulated sigmoid, redundant colon, advanced age, female gender, diverticular disease, and inadequate bowel preparation. In an effort to overcome these situations and to and aiding colonoscope insertion with reducing pain, various methods have introduced. Like this review discusses ways to approach patients with technically difficult colons for achieving the successful cecal intubation.
INTRODUCTION
Colonoscopy is a common and established endoscopic procedure for the diagnosis and treatment of many large bowel disorders including colorectal neoplasms. However, many people still regard it as an inconvenient and tough procedure, and colonoscopy sometimes cause some degree of pain even by an experienced endoscopist in the case of angulated and redundant colon. Endoscopists have put in an effort to improve the cecal intubation rate and to shorten the examination time with reduced discomfort. Despite these efforts, some cases of colonoscopy are more challenging than others, and incomplete colonoscopy commonly increases healthcare costs and patient inconvenience by resulting in additional, probably less sensitive, examinations like barium enema and virtual colonography.
"Difficult" is a subjective individual experience, and the actual definition may vary among endoscopists. Most commonly, we speak of a "difficult colonoscopy" as one in which it is challenging or impossible to reach the cecum. Others might be inclined to measure difficulty based on the duration of time required, the amount of physical exertion involved, or even the discomfort the patient experiences.
WHEN AND HOW DIFFICULT COLONOSCOPY OCCURS?
Quality indicators of the technical performance of colonoscopy
There has been an increasing emphasis on the quality of colonoscopy. Quality evaluation of the colon consists of intubation of the entire colon and a detailed mucosal inspection. Achieving safe cecal intubation improves the sensitivity of diagnosis and can eliminate the need for additional examination or a second colonoscopy to complete study. The United States Multisociety Task Force on Colorectal Cancer set an overall target of 90% for cecal intubation, with a goal of 95% in screening cases.1 In up to 10% to 20% of colonoscopies, intubation of the cecum may be considered difficult. US data report completion rate of gastroenterologists at academic centers ranging from 88% to 97%, with community gastroenterologists reporting similar percentages.2 In Korea, most reports showed relatively higher intubation rates (>90% to 95%) than those of Western countries. In other words, about 5% to 10% of cases were defined as a "difficult colonoscopy."
Risk factors for difficult colonoscopy
The overall technical skill of endoscopists is the foremost risk factor for difficult colonoscopy. Technical skill includes his or her innate manual dexterity, degree of formal training, and personal experience. Our multicenter trial objectively showed that a trainee's colonoscopy success rate depends on the number of colonoscopies completed. The success rate significantly improved and reached the requisite standard of competence (>90%) after 150 procedures.3 Other institute in Korea also showed results reaching more than 90% of cecal intubation rate after 200 procedures without senior supervisor.4 Several studies found that a prolonged cecal intubation time was associated with advanced age, female gender, low body mass index, poor quality of bowel preparation, and diverticular disease (Table 1).5,6 In addition, factors associated with prolonged cecal intubation for typical trainees did not differ from those for experienced colonoscopists.3
Loops or angulations in the colon are possibly the most common patient-related source of difficulty. Strictures, diverticulosis, and excess air insufflations during insertion can cause additional looping and angling because the expanded colon causes sharper angulation. Some bends require additional skill to navigate. Loops, particularly in the sigmoid colon, can result in loss of control of the endoscope as well as patient discomfort. Diverticular disease also increases the degree of difficulty; because a colon with severe diverticulosis can be more spastic, luminal narrowing and fixation can be more difficult to achieve adequate preparation, more difficult to insufflate, and more challenging to find the lumen safely. A study showed women with diverticular disease were 1.7 times more likely to require more than the median time to intubate the cecum.7
The quality of the preparation can make a great difference in the ease or difficulty of advancing the endoscope. Previous studies found the time required for cecal intubation was strongly associated with the quality of bowel preparation. In the article by Bowles et al.,8 poor bowel preparation was cited as the cause of 19.6% of failure to achieve complete colonoscopy. Also the patient's body habitus affects the degree of difficulty. It is certainly more difficult to apply counter-pressure on an obese abdomen to minimize looping. However, having a low body mass can result in an incomplete examination as well, with speculation that this is related to the paucity of visceral fat or the smaller abdominal cavity in which to fold the colon. Several studies have confirmed that colonoscopy is more difficult to perform in women and that there is anatomical sex differences in the colon. The female colon is longer, with a transverse colon 8 cm longer than the male colon on average and more frequent dips into the pelvis. The female colon is therefore more likely to be acutely angulated and tortuous. There is also a greater potential for angulation as the colon emerges from the pelvis, over the uterus, and into the left lower quadrant.
The impact of some factors is controversial. The results of several studies suggest that colonoscopies in women with prior hysterectomies may be more difficult compared with patients who have not had this operation.9,10 However, another study demonstrated that hysterectomy was no longer significantly related to a requirement for more than the median time for women to intubate the cecum after controlling for age. In addition, pelvic surgery such as cesarean sections or tubal ligation also did not affect time for cecal intubation.7
OVERCOMING DIFFICULT COLONOSCOPY
Using basic examine techniques
It is important for endoscopists to pay attention to loops and to minimize their formation by adequate endoscopic techniques such as hooking, torque, jiggling, pull back, and suctioning excess air. In patients with redundant colons, strict attention to proper fundamental colonoscopy technique, without resorting to special equipment or special colonoscopies, resulted in successful cecal intubation in three fourths of patients.11 In addition, properly applied abdominal pressure and position change can also help successful cecal intubation in the redundant and angulated colon.
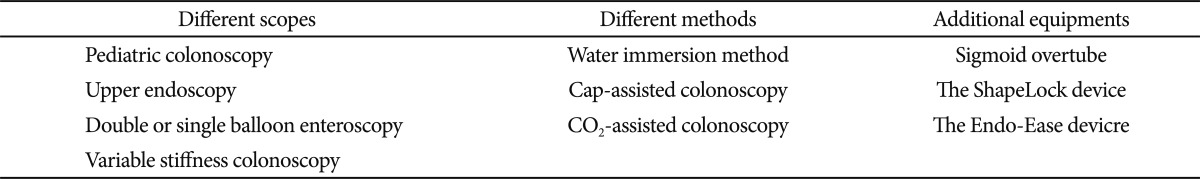
Different scopes
Pediatric colonoscopy was basically made for children. However, it has proved to be valuable in adult colonoscopy, not only for passing strictures but also where either fixation due to diverticular disease, postoperative adhesions, or unavoidably painful looping made passage impossible because the narrow diameter and greater flexibility seemed to allow forward movement.12,13 Pediatric colonoscopes have insertion tube diameters about 2 mm smaller than those of standard colonoscopes. These scopes are usually used first for patients with a very difficult sigmoid colon. However, even pediatric colonoscopies are often associated with more difficulty in advancement though the proximal colon due to excessive looping.
If a pediatric colonoscope cannot be passed through a narrowing or angulation, an upper endoscope will almost invariably pass benign angulations. An 8.6-mm-diameter upper endoscope has an insertion tube cross-sectional surface area that is 54% less than that of a standard colonoscope, and the bending section is shorter and has a tighter turning radius compared with standard colonoscopes. The upper endoscope often needs straightening combined with abdominal pressure for loop reduction and successful cecal intubation because of shorter length and flexible shaft. In a retrospective study on patients whose colonoscopy insertion failed twice, procedure was completed in 15 (51.7%) out of 29 cases by shifting to a standard gastroscope.14
An alternative to these techniques for dealing with an angulated sigmoid colon is to use a long endoscope with a diameter equivalent to that of a thin upper endoscope, such as a double balloon endoscope (diameter, 8.5 or 9.4 mm; length, 200 cm). Double balloon endoscope is a new technique for examination of the small intestine. The entire colon can be shortened and evaluated by the push and pull technique. A recently study demonstrated 88% of completion rate with this scope in previous incomplete colonoscopy.15 If a patient is referred with a known redundant colon, many prefer the variable stiffness device, although this preference lacks literature support. This device can pass sigmoid colon with the instrument shaft in the flexible mode followed by straightening of the instrument shaft.
Different methods
Water immersion is an alternative colonoscopy technique that may reduce discomfort and facilitate insertion of the instrument, help to straighten the tortuous sigmoid colon and open the lumen. Leung et al.16 reported that this technique leads to decreases in discomfort, time to reach the cecum, and amount of sedative and analgesic used without compromising patient satisfaction. In a recent study comparing air insufflation with water infusion method, the median maximum pain score (0=none; 10=most severe) during colonoscopy was significantly lower in the water group (3 vs. 6; p=0.004), and the cecal intubation rate with unsedated colonoscopy was significantly higher in the water group (98% vs. 78%). This report also showed that the water method enables increasing overall detection rate of adenoma and less than 10 mm hyperplastic polyps in the proximal colon.17 However, there is no report showing that the water-filling method can increase successful intubation rate in difficult colonoscopy cases. The method of utilizing CO2 gas instead of air insufflation was demonstrated in several studies. This method decreased pain scores and increased the proportion of patients with no pain after colonoscopy. The mechanism is based on rapid absorption of CO2 from the lumen, decreasing distention and associated pain.18 Several researchers have reported the effectiveness of a transparent hood for salvage in difficult cecal intubation.19,20 Kondo et al.19 reported that the transparent hood was useful, especially for inexperienced endoscopists, in terms of shortening the cecal intubation time, especially in difficult cases such as those involving elderly and female patients. In addition, the attachment of a hood to a conventional colonoscope is obviously less costly and easier to apply compared with other specialized endoscopes.
Simple sigmoid overtubes can be successful if looping occurs in the sigmoid colon. Sigmoid overtube (Olympus, Center Valley, PA, USA) manufactures a 60-cm reusable black flexible tube that has been used successfully in previously incomplete colonoscopies.11 The ShapeLock device (USGI Medical, San Clemente, CA, USA) is a highly sophisticated metal overtube that is flexible when initially inserted into the gastrointestinal tract and can be made rigid when desired. This device, in lengths of 60 and 80 cm, reportedly provides successful sigmoid straightening in previously incomplete colonoscopies.21 Another device that may have value in this setting is the Endo-Ease (Spirus Medical, Stoughton, MA, USA). This device is an overtube with a plastic spiral screw on it. The scope and straightener are advanced as a unit by a "screwing" action.22
Approach strategy
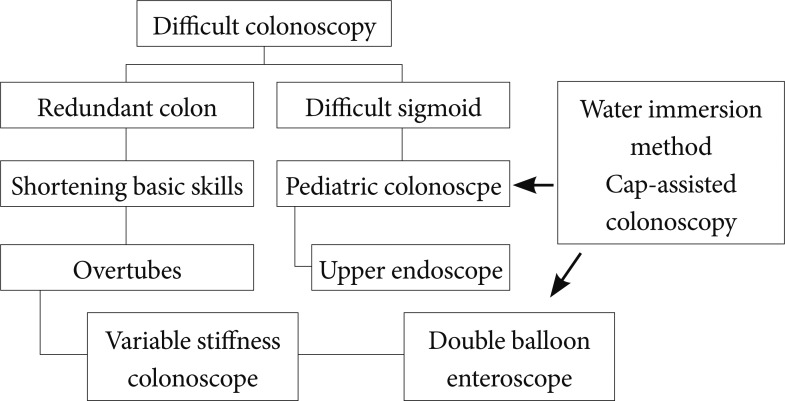
We have reviewed various tools for overcoming difficult colon including the different scopes and different methods (Table 2). In summary, the anatomic cause of difficult colonoscopy can usually be categorized into one of two problems: 1) angulated and/or narrowed sigmoid colon, or 2) redundant colon. This classification leads directly to the most appropriate approach to colonoscopy in these patients, as described in Fig. 1.
CONCLUSIONS
If colonoscopy is to be the true gold standard for prevention of colon cancer, complete visualization and removal of abnormal tissue must be ensured. This begins with meeting, or ideally exceeding, the set goals of 90% to 95% cecal intubation. It is important that the endoscopists have to pay attention to minimize loop formation by basic examine technique like adequate endoscopic skill, abdominal pressure, and position change. However, some patients may be inherently more difficult to intubate completely. In these cases, emerging technologies will provide additional help with difficult cases and enable endoscopists to handle even the most challenging colons with relative ease.
Notes
The authors have no financial conflicts of interest.