INTRODUCTION
A sufficient resection margin is recommended for complete resection of malignant tumors and reduction of the risk of residual tumor or recurrence. Especially in patients with adenocarcinoma in the gastrointestinal (GI) tract, survival can be affected by tumor recurrence from a microscopic residual tumor in the resection margin. Therefore, surgical resection of adenocarcinomas in the GI tract is recommended to close the abdomen after confirmation of the tumor-negative pathologic margin in frozen sections.
On the contrary, the interpretation of the pathologic margin in GI sarcomas such as gastrointestinal stromal tumor (GIST) is controversial. Unlike adenocarcinomas, GI sarcomas could show no significant difference in tumor recurrence or survival between the group with a negative pathologic margin and with a positive pathologic margin even though no residual tumor is visible. Little is known about R1 resection of GISTs from a retrospective institutional analysis with a small sample. Herein, the treatment strategy for GIST will be discussed with the interpretation of pathologic margins.
TREATMENT STRATEGY FOR GIST ACCORDING TO PATHOLOGIC MARGIN
Although a tumor-negative pathologic margin is commonly assumed to mean curative endoscopic or surgical resection of the malignant tumor, well-designed prospective randomized data to support this assumption are lacking. However, patients with residual sarcoma due to incomplete resection (R2) show poor clinical outcomes when compared with patients with R0 resection or even a microscopically positive resection margin (R1 resection) [1].
A microscopic positive margin has been reported to possibly have no influence on the disease-free survival of patients or even tumor recurrence in GIST [2]. In general, limited resection is recommended for achieving results comparable with those of extended resection. Surgical resection should include a margin of at least 1 cm of normal tissue and an intraoperative evaluation of frozen section [3]. In endoscopic resection, a sufficient vertical resection margin cannot be achieved for GISTs, which are located in the muscularis propria layer. As endoscopic submucosal dissection can only dissect the layer beneath the GIST, the resection margin may still involve by tumor cells irrespective of the completeness of the resection. If endoscopic full-thickness resection is performed, R0 resection can be achieved as well as surgical resection. A positive resection margin has been reported as ineffective for predicting the recurrence of small GISTs [4].
In a previous study that evaluated the risk of recurrence in R0 and R1 resection cases, recurrence-free survival was not significantly different between the two groups [5]. R1 surgical resection was associated with large tumor size and tumor rupture, and the risk of recurrence was associated with tumor rupture.
As the interpretation of pathologic margin is influenced by tumor contraction and fixation after resection, it can be affected by various factors during the process of tissue preparation. Therefore, R1 resection does not always mean incomplete resection because a false-positive margin may be assessed based on tissue contraction, encapsulation, or tumor rupture.
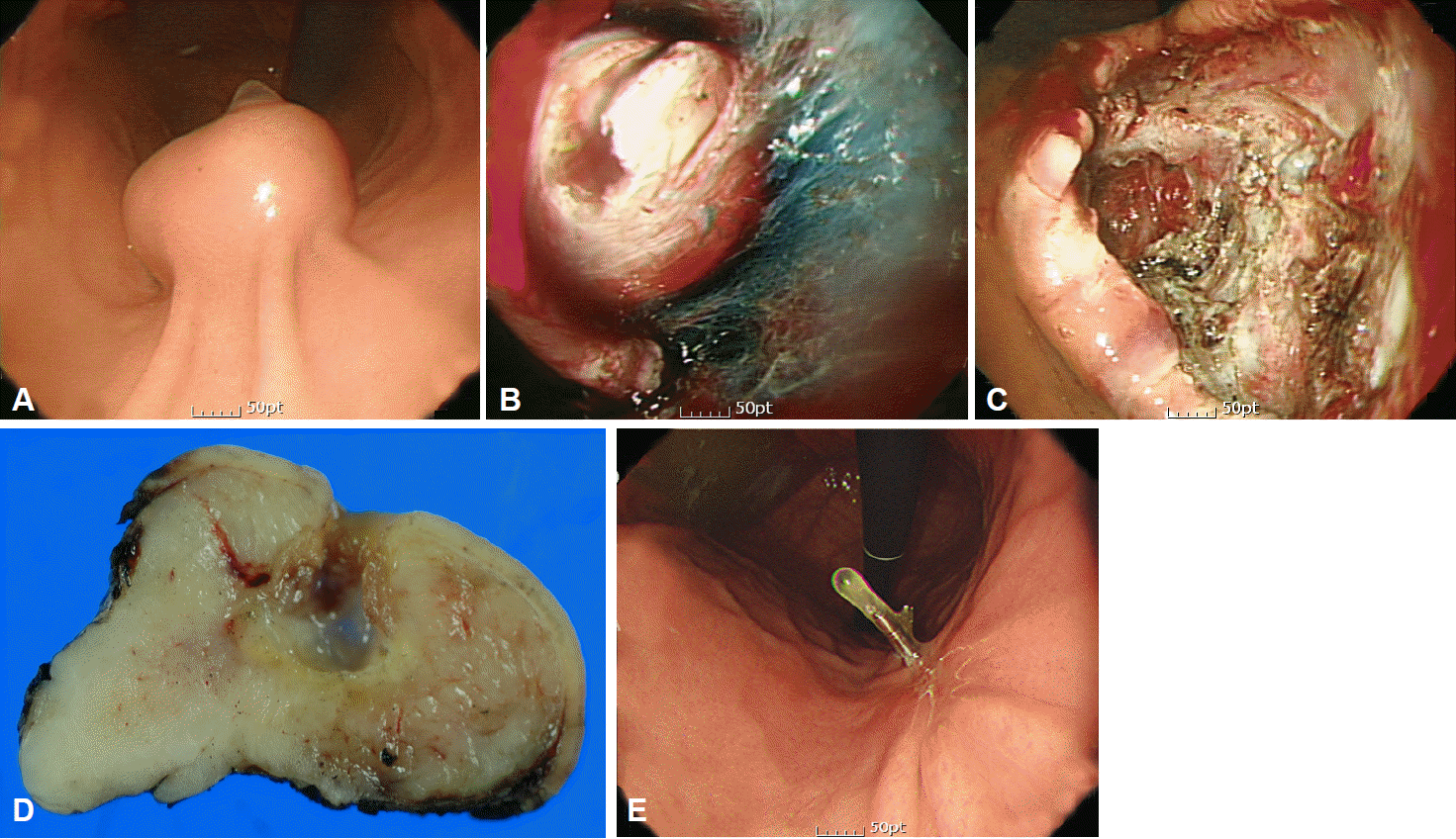
R1 resection is more frequent in endoscopic resection than in surgical resection because a sufficient resection margin is difficult to attain in endoscopic resection. In a recent study that compared endoscopic and surgical resections of GIST, R1 resection was more frequent in the endoscopic resection group than in the surgical resection group [6]. However, the recurrence rate with R1 resection in the endoscopic group was low (2.9%, 2/69), but not significantly different from that in surgical resection. Although the sample size of endoscopic resection cases was not sufficient to demonstrate the safety of R1 resection, it may be proposed that close serial follow-up can be useful if endoscopic resection is performed without evidence of residual tumor in spite of a microscopically tumor-positive resection margin (Fig. 1). These findings are consistent with those of a previous study that concluded that tumor size and not a microscopically tumor-positive margin was associated with disease-specific survival [7]. Therefore, serial endoscopic follow-up is recommended for GIST cases with R1 endoscopic resection if no residual tumor is evident immediately after endoscopic resection. As residual or recurrent tumor is possible, close follow-up is mandatory for patients who undergo R1 resection.