INTRODUCTION
The treatment of choice for acute cholecystitis is laparoscopic cholecystectomy; however, this procedure is unsuitable for patients who are critically ill and have significant comorbidities [1]. In such patients, percutaneous cholecystostomy (PC) is an effective alternative option, as it is a safe and minimally invasive radiologic procedure with which immediate gallbladder decompression and prompt clinical improvement are possible. The technical success rate and clinical response rate associated with PC has been reported to be up to 100% and 95%, respectively [2-4]. However, long-term placement of a PC tube has several disadvantages, such as patient discomfort, the need for repeated procedures, and catheter dislodgement [4,5]. In addition, the recurrence rate of cholecystitis after removal of the PC tube has been reported to be 33%ŌĆō41% in previous studies [2].
Endoscopic transpapillary gallbladder stenting (ETGS) is another alternative option. With this procedure, internal drainage can be performed and the patientŌĆÖs quality of life can be preserved. ETGS requires biliary and cystic duct cannulation. During ETGS, the guidewire is advanced retrogradely into the gallbladder, which is the most challenging part of the procedure. However, in patients who have already undergone PC, the guidewire can be advanced antegradely through the gallbladder into the duodenum, which improves the success rate of cystic duct cannulation. Herein, we report the case of a patient who initially underwent PC for severe acute cholecystitis and, after recovery, underwent successful conversion to ETGS with the rendezvous technique.
CASE REPORT
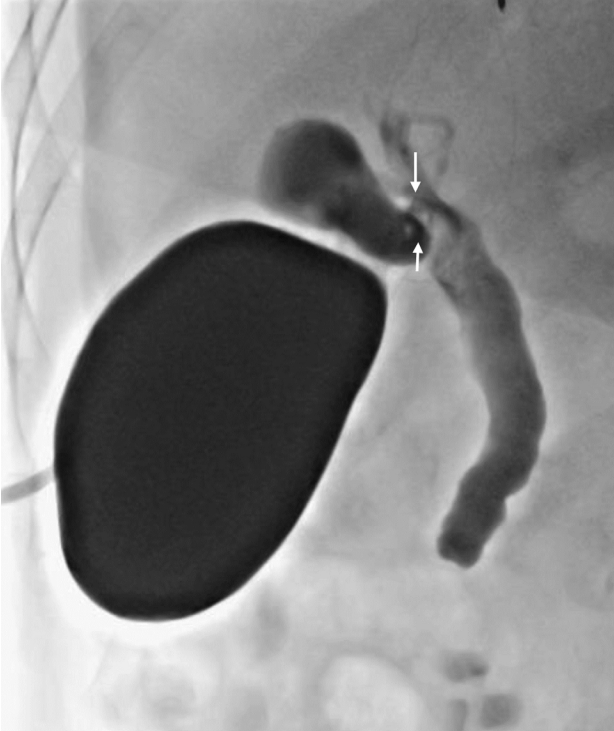
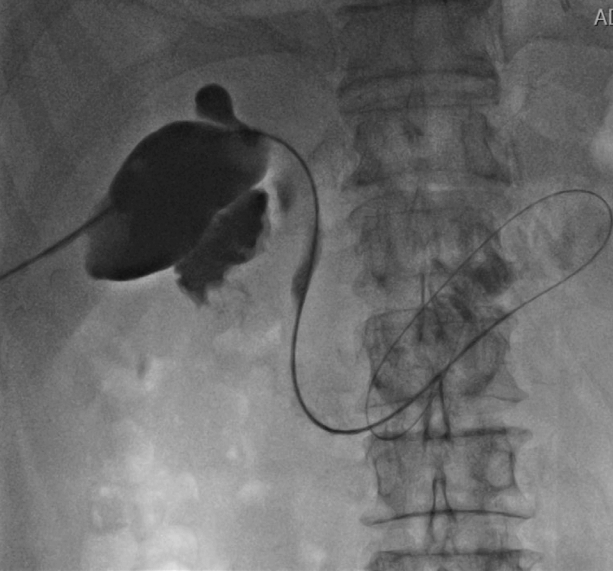
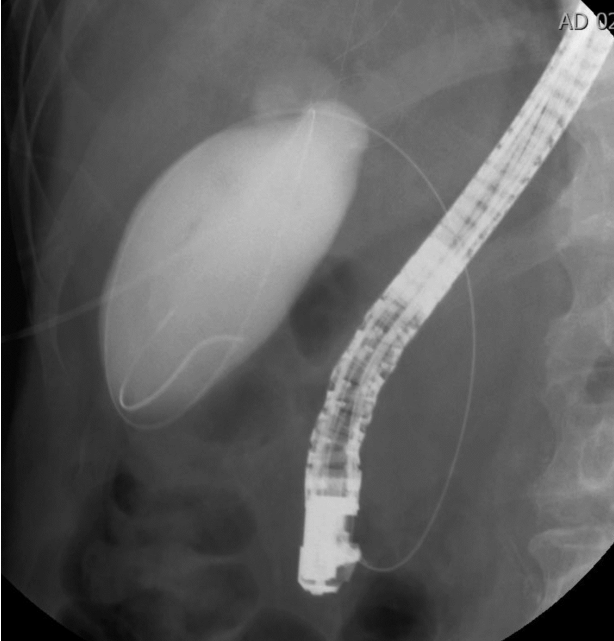
An 84-year-old man with diabetes and severe coronary artery disease came to our hospital with a complaint of right upper-quadrant pain. He developed severe acute cholecystitis complicated by sepsis, and hemodynamic instability. He underwent emergent PC, which resulted in clinical improvement. After his condition improved, we considered removing the PC tube. However, abdominal pain recurred immediately after the PC tube was clamped. Given the high surgical risk associated with his condition, endoscopic retrograde cholangiopancreatography for ETGS was performed 1 week later. Selective cannulation of the cystic duct was attempted; however, it was unsuccessful, even after guidewires of various sizes and papillotomes such as Autotome (Boston Scientific, Microvasive, Marlboro, MA, USA), were used, because of cystic duct stricture and tortuosity (Fig. 1). To facilitate cystic duct access, the cholecystostomy tube was replaced with a hydrophilic guidewire that was passed antegradely into the duodenum (Fig. 2). Then, a duodenoscope (JF-260V; Olympus Medical Co., Tokyo, Japan) was inserted up to the papilla, at the point where the guidewire was coming out. The guidewire was grasped with forceps and pulled out through the accessory channel of the duodenoscope. Cystic duct cannulation was achieved with a cannula placed over the antegradely placed guidewire (Fig. 3). Finally, a 7-F, 12-cm-long double-pigtail plastic stent (Cook Medical, Bloomington, IN, USA) was advanced over the wire with one loop left in the gallbladder and one in the duodenum (Fig. 4). The percutaneous catheter was removed after the procedure. Cholecystitis did not recur, and the patientŌĆÖs condition remained stable during the 17-month follow-up.
DISCUSSION
Selective deep cannulation of the cystic duct is essential for a successful ETGS. However, even the most experienced endoscopists fail in cannulating the cystic duct in 21% of cases [6]. When a selective cystic duct cannulation fails, PC allows successful immediate gallbladder drainage and retrograde access for a subsequent rendezvous technique [7-11]. This combined technique increases the success rate of cystic duct cannulation and facilitates the placement of a gallbladder stent. We report the case of a patient who had initially undergone emergent PC and, after clinical improvement, underwent successful conversion to ETGS with the rendezvous technique. The guidewire was anterogradely placed through the PC tract to the duodenum, and a double-pigtail plastic stent was retrogradely inserted by using the transpapillary approach. The patient had no recurrent cholecystitis during the 17-month follow-up period.
In patients who develop severe acute cholecystitis but are medically unfit for cholecystectomy because of significant comorbidities, emergent PC is the treatment of choice. After clinical improvement, however, long-term placement of the PC tube is troublesome. Furthermore, simple removal of the PC tube may lead to frequent recurrence of cholecystitis [2]. In this situation, ETGS after PC should be considered. Because transmural puncture is not performed during the procedure, the risk of bile leakage, bile peritonitis, and bleeding is low [12]. ETGS can be used as a bridge therapy (if elective cholecystectomy is scheduled) or as a definite therapy (if there is a contraindication to elective cholecystectomy) [6,7,13,14]. A double-pigtail plastic stent can preserve cystic duct patency and prevent recurrent cholecystitis. After stent placement, a ŌĆ£wait-and-seeŌĆØ approach is recommended, because continuous bile drainage is possible along the occluded stent (the ŌĆ£wicking phenomenonŌĆØ) [6,15]. In a long-term follow-up study, a mean stent patency of 760 days was reported without regular stent change [6].
The main drawback of ETGS is its lower success rate than that of PC. The technical success rate and clinical response rate have been reported to be 96% and 88%, respectively, which are lower than those of PC. This is mainly due to the difficulty associated with cystic duct cannulation. In cystic duct cannulation, the guidewire maneuver is difficult because of the corkscrew shape and narrowness of the cystic duct, as well as the presence of the spiral valve of Heister. In addition, the cystic duct may show stricture or obstruction in acute cholecystitis [7]. In the present case, cystic duct stricture and tortuosity were also found in the cholecystogram (Fig. 1), which were associated with failure of cystic duct cannulation through the transpapillary approach. However, by using the PC tract, antegrade guidewire insertion into the duodenum was more easily performed because there was enough space for guidewire manipulation. After the successful ETGS placement, the PC tube was removed and there was no bile leak after tube removal.
Several cases of percutaneous transgallbladder rendezvous for ETGS placement have been reported. Elmunzer et al. reported on 2 patients who underwent PC for severe acute cholecystitis and, after recovery, underwent ETGS with the guidewire advanced through the cholecystostomy tract into the duodenum [15]. During the long-term follow-up period (10 and 6 months of follow-up), the patients remained stable. Maekawa et al. reported on 5 patients who underwent ETGS by passing the guidewire antegradely into the duodenum via the PC route and then by using the guidewire retrogradely [7]. The success rate of the procedure was 100% (5 of 5) and was higher than that of emergent ETGS (77.5%, 31 of 40). Hatanaka et al. reported on 2 patients with unresectable cancer who had undergone PC because of failed ETGS, and then underwent a successful ETGS with a rendezvous approach [8]. During the rendezvous procedure, a PC-placed guidewire was grasped at the tip of the duodenoscope; then, the duodenoscope and wire were withdrawn. In case of difficulty in grasping the wire with forceps, Matsubayashi et al. suggested a parallel cannulation technique along with PC rendezvous [9]. A modified rendezvous technique in which the guidewire was retrogradely passed into the gallbladder after end-to-end contact between the tips of the sphincterotome and the PC catheter at the orifice of the ampulla may also be a feasible option [16]. However, extending a PC tube into the duodenal lumen is often difficult.
In conclusion, conversion of PC to ETGS is a viable option in patients with acute cholecystitis who are unfit for cholecystectomy. Antegrade guidewire insertion via the PC tract and subsequent ETGS placement by using the rendezvous technique may increase the success rate and decrease the risk of procedure-related complications. However, further studies are needed to evaluate the feasibility of conversion with antegrade guidewire insertion in patients with acute cholecystitis and severe comorbidities.