Primary splenic malignant lymphoma is very rare, and few reports have examined the diagnostic utility of endoscopic ultrasound-guided fine-needle biopsy (EUS-FNB) for this disease [1-3]. Here we report an extremely rare case of hepatosplenic T-cell lymphoma (HSTCL). Although HSTCL has been previously documented in patients with inflammatory bowel disease [4,5], this is the first report of it being diagnosed by splenic biopsy using EUS-FNB. HSTCL is an extranodal cytotoxic T-cell lymphoma that is located in the liver or spleen, and easily invades the bone marrow; it is characterized by marked hepatosplenomegaly and B symptoms. This disease is more common in young men, and has an aggressive course and poor prognosis [6,7].
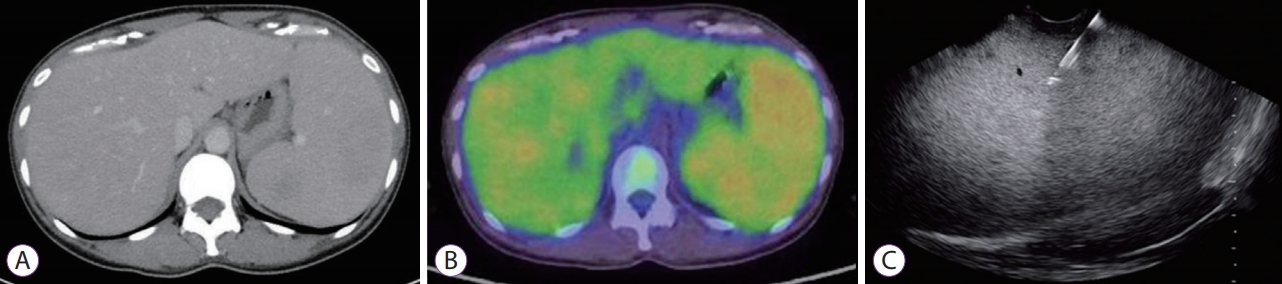
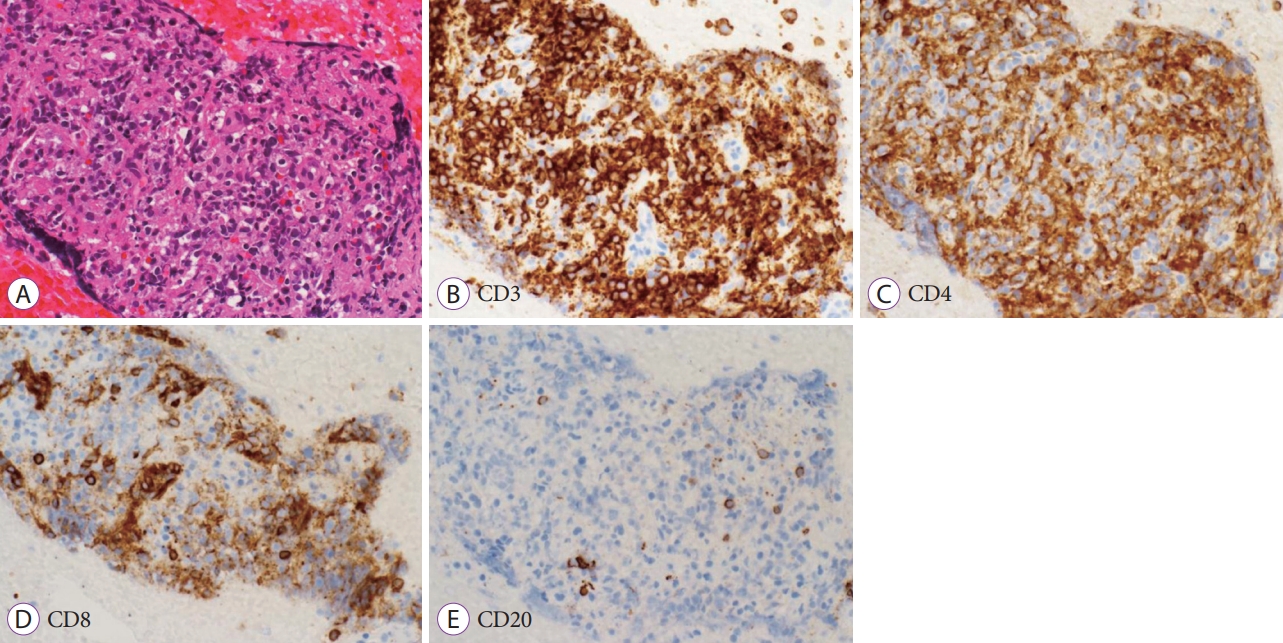
The patient was a 44-year-old woman who was admitted to our hospital with complaints of fever and abdominal pain. Hematologic examination revealed thrombocytopenia, a prolonged blood coagulation time, and an increased serum lactate dehydrogenase level. The platelet count was 73,000/mm3 (normal range, 158,000ŌĆō348,000/mm3), the international normalized ratio of prothrombin time was 1.37 (normal range, 0.85ŌĆō1.15), the activated partial prothrombin time was 47.1 sec (normal range, 20.0ŌĆō40.0 sec), and the serum lactate dehydrogenase level was 593 IU/L (normal range, 124ŌĆō222 IU/L). Abdominal computed tomography (CT) showed marked splenomegaly (Fig. 1A). 18F-Fluorodeoxyglucose (F-FDG) positron emission tomography/CT showed preferential accumulation of 18F-FDG in the spleen (Fig. 1B), as well as in the liver and bone marrow, but there was no accumulation in the lymph nodes. EUS revealed that the spleen was markedly enlarged, with small isoechoic to hypoechoic areas throughout, but no noticeable mass formation was observed (Fig. 1C). The decision was made to perform EUSFNB to confirm a suspected diagnosis of splenic lymphoma. Written informed consent was obtained from the patient after providing a detailed explanation of the procedure. The splenic lesion was punctured transgastrically (Fig. 1C) and the tissue was collected under slight negative pressure using the slow-pull method by slowly withdrawing the stylet [8,9]. Five punctures were performed using a 22-gauge reverse bevel FNB needle (EchoTip ProCore; Cook Medical, Bloomington, IN, USA) to obtain tissue for immunohistochemistry analysis. There were no procedure-related adverse events. Histopathologic analysis showed diffuse infiltration of medium-sized atypical lymphocytes, with clear cytoplasm, into the sinusoids of the spleen (Fig. 2A). Immunohistochemistry analysis revealed markedly abnormal lymphoid infiltrates in the splenic sinuses that were positive for CD3 (Fig. 2B) and negative for CD4 (Fig. 2C), CD8 (Fig. 2D), and CD20 (Fig. 2E), which is characteristic of HSTCL. The results of bone marrow analysis using flow cytometry also supported this diagnosis, and this case was found to be of the ╬▒╬▓ T-cell receptor type (with the ╬▒╬▓ type being less dominant than the ╬│╬┤ type) [6,7]. Using a 22-gauge core biopsy needle allowed the collection of a tissue sample with a length of 579.4 ┬Ąm, which was sufficient to meet the fifth criterion (sufficient material for good quality histological interpretation) in the standard microscopic scoring system proposed by Gerke et al. [10]. A 19-gauge core biopsy needle is useful for diagnosis of splenic malignant lymphoma by EUS-FNB because a large amount of tissue can be collected with a small number of punctures [2,3], but procedures involving an EUS scope sometimes require a strong upward angle and rightward torque to detect and puncture splenic lesions. A 22-gauge biopsy needle is more flexible than a 19-gauge needle, therefore less resistance is encountered when attaching the needle and puncturing the target in such situations. This makes it easier for less experienced operators to control the needle and puncture the target. Therefore, we opted to use a 22-gauge core biopsy needle for splenic biopsy in this case.
The spleen is the primary site of non-HodgkinŌĆÖs lymphoma in only 1%ŌĆō3% of the cases [6,7]. Furthermore, HSTCL accounts for less than 1% of all non-HodgkinŌĆÖs lymphomas [6,7]. Interestingly, 10% of the known cases of HSTCL have been documented in patients with inflammatory bowel disease, such as CrohnŌĆÖs disease or ulcerative colitis [4,5]. There have also been some reports of cases where immunosuppressants, such as anti-tumor necrosis factor (TNF) and thiopurine, have been used in combination [4,5]. Concomitant use of thiopurine and anti-TNF is thought to cause bone marrow suppression, resulting in an inability to selectively control cell proliferation and development of HSTCL via a genetic mechanism [4]. Our patient did not have a history of inflammatory bowel disease or immunosuppressive therapy. Immunosuppressants such as anti-TNF and thiopurine are now widely used in inflammatory bowel disease, and patients receiving these agents should be monitored carefully for development of HSTCL. Splenic biopsy with EUS using a core biopsy needle, which is a minimally invasive procedure, may aid in early diagnosis of HSTCL in patients with inflammatory bowel disease receiving immunosuppressive therapy.