INTRODUCTION
Mucormycosis (previously called zygomycosis) is a rare and devastating disease caused by a ubiquitous fungus that belongs to the class Zygomycetes and order Mucorales [1]. The clinical presentation of mucormycosis varies depending on the location of the disease [2]. The majority of patients with invasive mucormycosis are either undergoing treatment with immunosuppressants or have underlying conditions, such as diabetes mellitus, hematologic malignancies, and trauma or are transplant recipients. Outbreaks of the fungal disease have also been associated with natural disasters [3-5].
Although unusual, mucormycosis of the gastrointestinal (GI) tract occurs as a result of the ingestion of the spores of the fungus. Cases of GI mucormycosis in an immunocompetent host are rarely reported; however, the mortality rate due to GI mucormycosis can be as high as 85% [6].
In early December 2019, the first cases of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection were identified in Wuhan [7,8]. As this is a relatively novel virus, data regarding all the signs indicative of coronavirus disease (COVID-19) and symptoms that can be caused by the disease are insufficient [9]. Furthermore, little is known about other diseases that can increase the risk of SARS-CoV-2 coinfection. To the best of our knowledge, this is the first case of mucormycosis reported in a COVID-19 patient.
CASE REPORT
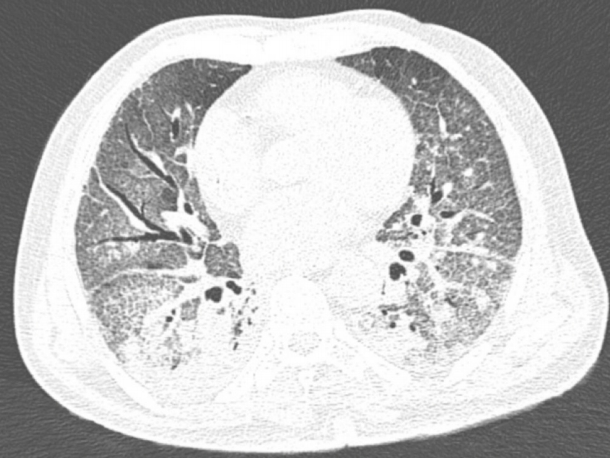
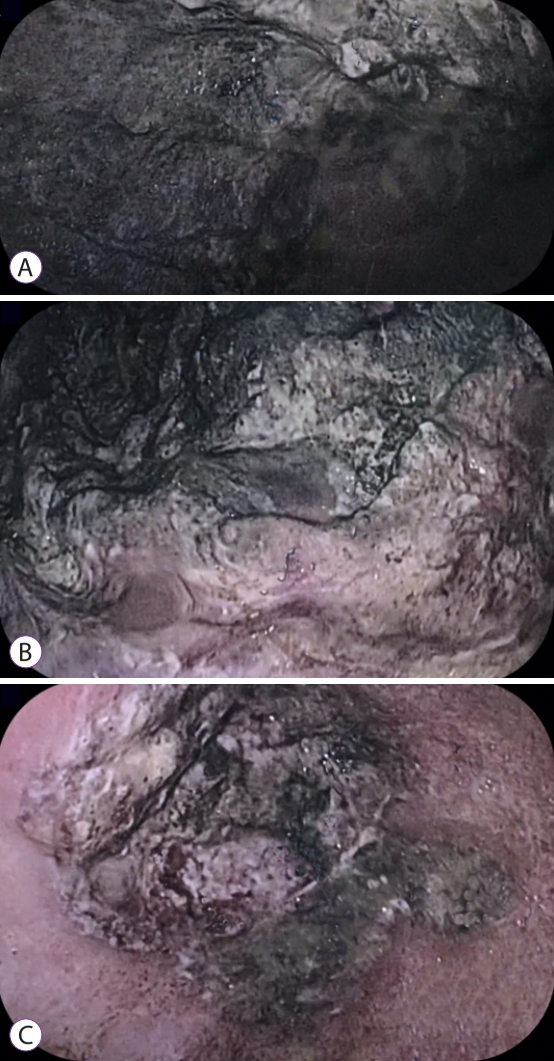
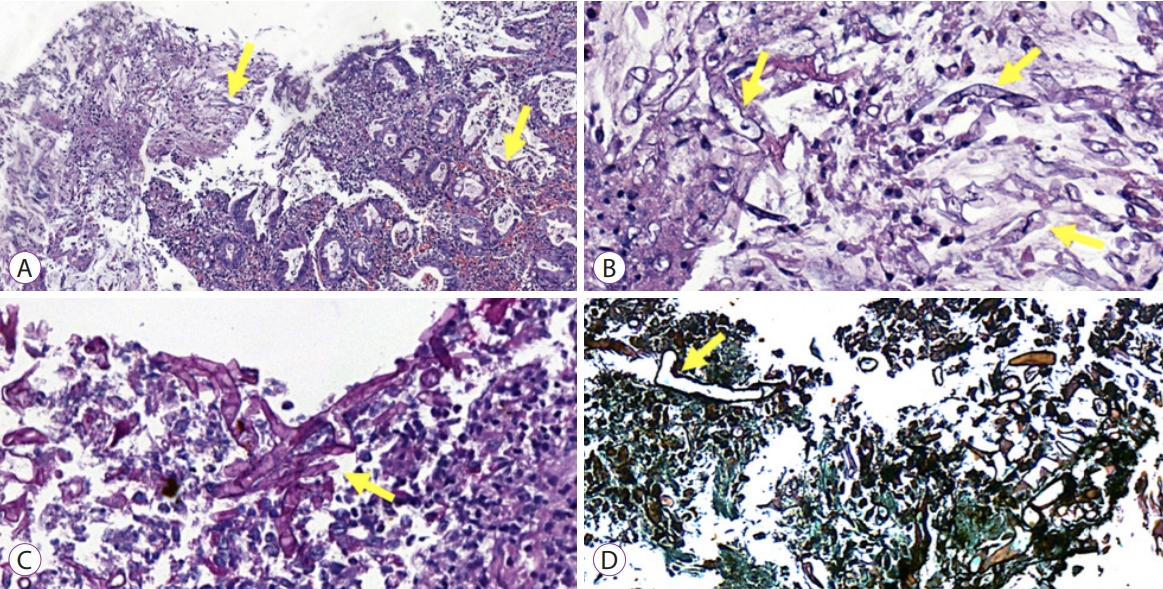
An 86-year-old male patient with a history of arterial hypertension was admitted to the emergency room with acute diarrhea, cough, dyspnea, and fever that started 5 days before admission. Blood analysis revealed a hemoglobin level of 14.3 mg/dL, a leukocyte count of 11.2Ć109/L, lymphocyte count of 0.58Ć109/L, a D-dimer level of 602 ng/mL, a lactate dehydrogenase level of 850 U/L, a creatinine level of 2.34 mg/dL, and a urea level of 93 mg/dL. A throat swab was collected from the patient, which confirmed COVID-19. Computed tomography of the chest was performed, and the findings are demonstrated in Fig. 1. Due to acute respiratory failure and hemodynamic instability, he was transferred to the intensive care unit (ICU). The patient was initially treated with ceftriaxone, azithromycin, oseltamivir, and hydrocortisone, besides intensive care management including vasopressors and mechanical ventilation. Five days following ICU admission, the patient presented with melena and severe anemia (hemoglobin level of 5.6 mg/dL). Physical examination revealed mild abdominal tenderness. He was managed with three units of red blood cells and omeprazole. Esophagogastroduodenoscopy (EGD) revealed two giant gastric ulcers with dirty debris and a deep hemorrhagic base without active bleeding located in the greater and lesser curvature (Fig. 2). Pathological examination confirmed mucormycosis (Fig. 3). Unfortunately, the patient died 1 week following hospitalization, 36 hours after the EGD, and before a diagnosis was established. Antifungal agents were not administered.
DISCUSSION
The ongoing outbreak of COVID-19 originated in Wuhan, China, in December 2019. COVID-19, which is the disease associated with SARS-CoV-2 infection, spread rapidly to produce a global pandemic [10]. The spectrum of symptomatic SARS-CoV-2 infection ranges from mild to critical. The proportion of severe or fatal infections may also vary by location.
Patients with COVID-19 might present with markedly higher levels of inflammatory cytokines (such as interleukin [IL]-2R, IL-6, IL-10, and tumor necrosis factor-alpha), associated with impaired cell-mediated immune response, affecting both CD4 + T and CD8 + T cells. Hence, an increased susceptibility to fungal coinfections is observed [11].
Mucormycosis is characterized by infarction and necrosis of the host tissues that result from an invasion of the vasculature by hyphae. Depending on the anatomic site involved, mucormycosis can present as a variety of different syndromes, including rhino-orbital-cerebral, pulmonary, cutaneous, and less often GI, renal, and disseminated diseases [12]. GI involvement presents in approximately 8% of the cases. The most commonly affected organs in the GI tract include the stomach and colon.
The symptoms of GI mucormycosis may include fever, nausea, abdominal pain, GI bleeding, and perforation. Establishing a correct diagnosis is challenging due to the nonspecific clinical signs/symptoms, which may not result in suspicions of mucormycosis. The endoscopic appearance of gastric mucormycosis is usually a large ulcer with necrosis, eventually presenting an adherent, thick, green exudate [13,14]. Diagnosis is confirmed by histopathologic identification based on the biopsy of the suspected area during surgery or endoscopy [6]. The disease has a high fatality rate (up to 85%) related to late or no diagnosis [15].
Treatment involves surgical debridement of involved tissues and antifungal therapy. Intravenous amphotericin B (a lipid formulation) is the drug of choice for initial therapy [16]. Despite early diagnosis and aggressive combined surgical and medical therapy, the prognosis for recovery from mucormycosis is poor [6].
We presented a case of an elderly patient whose only known comorbidity was arterial hypertension, without traditional risk factors for developing mucormycosis. He was admitted following the diagnosis of COVID-19 and acute respiratory failure and managed with broad-spectrum antibiotics and corticosteroids (which are risk factors for invasive fungal disease) [17]. It is known that COVID-19 may be associated with immune dysregulation [18], and it has been reported that patients with COVID-19 might be at risk of developing invasive fungal infections, such as invasive aspergillosis, candidiasis, and Pneumocystis jiroveci infection [11,19]. However, there are no reports of mucormycosis associated with COVID-19. Our patient was diagnosed with primary gastric mucormycosis, but it is unknown whether the cause of death was invasive mucormycosis.
GI mucormycosis is a rare disease, and it should be considered if an atypical gastric ulcer is identified in a COVID-19 patient. Clinical suspicion and prompt treatment are fundamental to achieve the cure of the disease. Hence, preemptive therapy should be considered in the presence of features suggesting mucormycosis. More studies are necessary to determine if these two pathologies are related.