Contamination Rates in Duodenoscopes Reprocessed Using Enhanced Surveillance and Reprocessing Techniques: A Systematic Review and Meta-Analysis
Article information
Abstract
Background/Aims
Multiple outbreaks of multidrug-resistant organisms have been reported worldwide due to contaminated duodenoscopes. In 2015, the United States Food and Drug Administration recommended the following supplemental enhanced surveillance and reprocessing techniques (ESRT) to improve duodenoscope disinfection: (1) microbiological culture, (2) ethylene oxide sterilization, (3) liquid chemical sterilant processing system, and (4) double high-level disinfection. A systematic review and meta-analysis was performed to assess the impact of ESRT on the contamination rates.
Methods
A thorough and systematic search was performed across several databases and conference proceedings from inception until January 2021, and all studies reporting the effectiveness of various ESRTs were identified. The pooled contamination rates of post-ESRT duodenoscopes were estimated using the random effects model.
Results
A total of seven studies using various ESRTs were incorporated in the analysis, which included a total of 9,084 post-ESRT duodenoscope cultures. The pooled contamination rate of the post-ESRT duodenoscope was 5% (95% confidence interval [CI]: 2.3%–10.8%, inconsistency index [I2]=97.97%). Pooled contamination rates for high-risk organisms were 0.8% (95% CI: 0.2%–2.7%, I2=94.96).
Conclusions
While ESRT may improve the disinfection process, a post-ESRT contamination rate of 5% is not negligible. Ongoing efforts to mitigate the rate of contamination by improving disinfection techniques and innovations in duodenoscope design to improve safety are warranted.
INTRODUCTION
Endoscopic retrograde cholangiopancreatography (ERCP) is an important lifesaving procedure for the diagnosis and treatment of hepatobiliary and pancreatic conditions. Duodenoscopes are used in over 500,000 ERCPs in the United States annually [1], and since 2012, more than 25 outbreaks with multidrug-resistant organisms have been reported worldwide due to patient cross-contamination attributed to duodenoscopes [2]. Currently, duodenoscopes used to accomplish most of the ERCPs are reusable, and owing to their intricate design, they are difficult to disinfect/sterilize. These factors have been implicated as the primary reason for the infectious outbreaks associated with their use [3].
In August 2015, the United States Food and Drug Administration (FDA) recommended enhanced surveillance and reprocessing techniques (ESRT) to improve duodenoscope disinfection. Along with the manufacturer-recommended manual cleaning and high-level disinfection (HLD) process, adding one of the following supplemental measures was recommended: (1) microbiological culture, (2) ethylene oxide (EtO) sterilization, (3) use of a liquid chemical sterilant processing system, and (4) repeat or double HLD (dHLD) [4]. Implementation of any of these ESRTs or a combination of techniques was dependent on an institution’s preference and availability of resources.
In October 2015, the FDA mandated all three major duodenoscope manufacturers (Fujifilm Medical Systems USA, Inc., Olympus Medical Systems Corporation, Pentax America) to conduct a post-market surveillance to analyze how duodenoscopes are processed in a real-world setting by sampling and culturing after the use of labeled reprocessing instructions. Preliminary results from these post-market surveillance studies as of July 2019 have shown a contamination rate of up to 5% with disease-causing high-risk organisms (HRO) (organisms that are more frequently associated with diseases) in patient-ready duodenoscopes [1,5,6]. However, if non-HRO are considered, studies have reported contamination rates as high as 13%–15% [7,8]. Many studies have evaluated the impact of ESRT by comparing different techniques versus each other or versus standard HLD [9–15]. No study has examined the combined effectiveness and contamination rates of all the ESRTs recommended by the FDA. A systematic review and meta-analysis was performed to assess the effect of ESRT on duodenoscope contamination rates.
METHODS
This systematic review was performed according to the Cochrane Handbook for Systematic Reviews of Interventions [16]. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were followed to report this study [17].
Search strategy
A comprehensive search was performed across multiple databases from inception to January 6, 2021. The search included studies only in the English language and excluded animal studies. The databases included Ovid MEDLINE® and Epub Ahead of Print, In-Process & Other Non-Indexed Citations and Daily, Ovid Embase, Ovid Cochrane Central Register of Controlled Trials, Ovid Cochrane Database of Systematic Reviews, and Scopus. The search strategy was devised by a qualified librarian and performed with feedback from the principal investigator of the study. Controlled vocabulary supplemented with keywords was used to search for articles describing the reprocessing or disinfection of duodenoscopes. The search strategy, which includes all the terms used in the search and their combinations, is presented in Supplementary Material 1.
The search was performed using a combination of keywords that included “duodenoscopes”, “disinfection”, “reprocessing”, “contamination”, “culture and monitoring”, “ethylene oxide”, “liquid chemical sterilant”, and “high-level disinfection”. Two authors independently reviewed the studies and abstracts included in the initial search and excluded those that did not address the outcome of interest. The full texts of the remaining articles were reviewed to ascertain if they contained pertinent information. The bibliographic sections of the chosen articles and narrative articles on the topic were reviewed and checked for further relevant studies. Any inconsistencies regarding the selection of articles were resolved after discussion with the senior author.
Selection criteria
In the current analysis, studies that reprocessed duodenoscopes using one of the four supplemental techniques recommended by the FDA were incorporated: (1) microbiological culture, (2) EtO sterilization, (3) use of a liquid chemical sterilant processing system, and (4) dHLD. Studies assessing the impact of these ESRTs and reporting the contamination rates of duodenoscopes after performing these techniques were included. In microbiological culture techniques, the frequency of microbial culturing and surveillance is not clearly defined by the FDA; hence, only studies that did culture and quarantine after each procedure and reprocessing before using it on a patient were included. Exclusion criteria were as follows: (1) studies that performed and assessed only manufacturer-recommended manual cleaning and HLD; (2) studies that did not report the contamination rates of duodenoscopes after ESRT; (3) animal studies and studies not in the English language; and (4) letters to the editor, review articles, case reports, and editorials. If there were multiple publications from an identical cohort, data from most current and/or most relevant comprehensive reports were included.
Data extraction and quality assessment
After relevant studies were identified, two authors (Shivanand Bomman, Navroop Nagra) extracted all the data on outcomes related to the studies on a standardized form. A modified Newcastle-Ottawa scale for cohort studies was utilized to assess the quality of each study by two authors (SB, NN) [18]. The quality assessment scale comprised seven questions, which included the following: (1) multicenter vs. single-center study; (2) study cohort size; (3) definitive information on HRO and non-HRO; (4) article type (abstract vs. manuscript); (5) type of study (retrospective vs. prospective); (6) duration of study; and (7) frequency of cultures (random vs. daily). Supplementary Table 1 provides the details of the quality assessment scale. With a maximum possible score of 10, a score of ≥8 was deemed high-quality, 6–7 was considered medium, and ≤5 was considered low-quality. Any inconsistencies in data extraction and assessment of study quality were resolved by a collaborative evaluation of the original articles by two authors (SB, NN).
Outcomes assessed
The pooled contamination rates of duodenoscopes after using ESRT, our primary outcome of interest, was calculated as the proportion of contaminated duodenoscopes with positive cultures relative to the number of duodenoscopes cultured. The secondary outcome of interest was to assess contamination rates with HRO, which are defined by the Centers for Disease Control as non-contaminant organisms more often associated with disease, such as Gram-negative bacteria (e.g., Escherichia coli, Klebsiella pneumoniae, or other Enterobacteriaceae, as well as Pseudomonas aeruginosa), Staphylococcus aureus, Enterococcus, and yeast [19].
Statistical analysis
The random effects model described by DerSimonian and Laird was used to evaluate the pooled contamination rates of duodenoscopes after ESRT with 95% confidence interval (CI) [20]. The inconsistency index (I2) was calculated to evaluate the heterogeneity among the study-specific estimates. I2 evaluates the proportion of observed variance due to heterogeneity instead of simply by chance. The calculated I2 values of <30% were considered low, 30%–60% considered moderate, and 61%–75% and >75% were considered to be suggestive of substantial and considerable heterogeneity, respectively [21]. A p value of <0.05 was considered statistically significant. Publication bias was planned to be ascertained using funnel plots and Egger tests if 10 or more studies were included in the meta-analysis. Statistical analyses were performed using Comprehensive Meta-Analysis software, version 3 (BioStat, Englewood, NJ, USA).
RESULTS
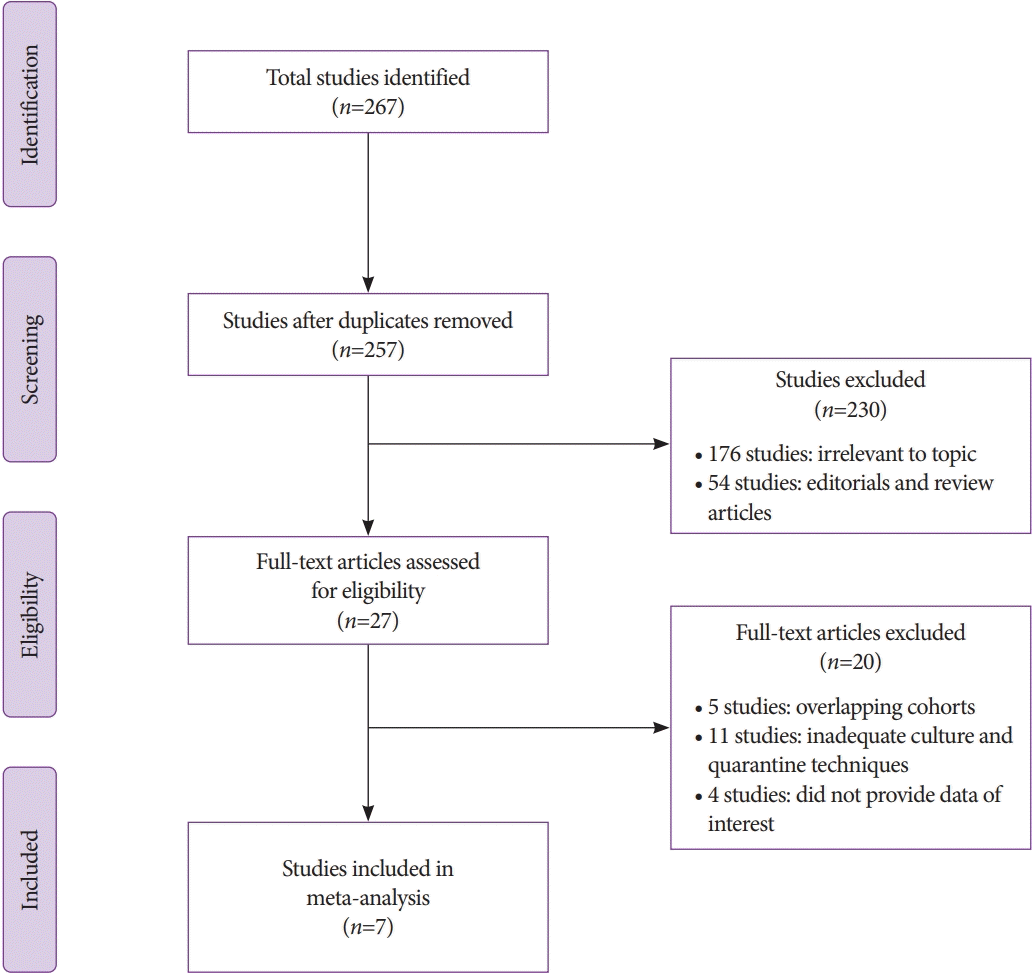
Our search criteria included 267 studies. Duplicates were excluded, and 257 studies were reviewed on the basis of the title and abstract. After eliminating 230 non-relevant studies on the basis of a review of titles and abstracts, 27 full-text articles were reviewed. Eleven studies were excluded due to inadequate culture and quarantine techniques, five studies had overlapping cohorts, and four did not report data of interest.
Seven studies reporting duodenoscope contamination rates after ESRT were included in the meta-analysis as they met the aforementioned inclusion criteria [9–15]. Fig. 1 illustrates the study identification and selection process.
Study characteristics
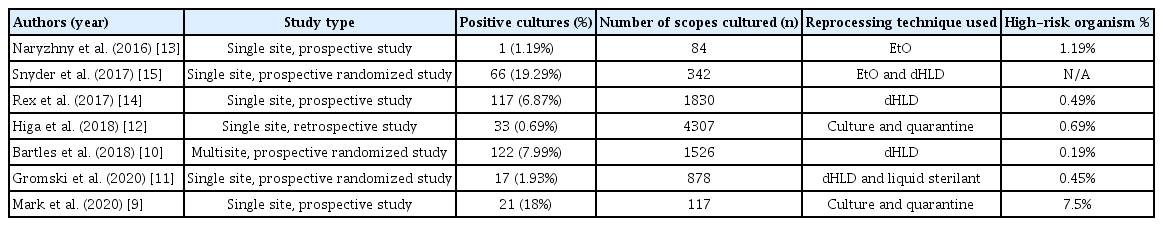
Table 1 summarizes the characteristics of all the included studies. One was a multisite study [10], and the remainder were single-center studies. Three were prospective randomized studies comparing different types of disinfection processes [10,11,15]. Three were prospective studies looking at contamination rates after one of the ESRTs [9,13,14]. One study was a retrospective data review of a prospectively collected database [12]. Two studies used culture and quarantine method [9,12]; two used dHLD method [10,14]; one study used EtO sterilization [13]; one used either EtO or dHLD [15]; and one study used either liquid sterilant or dHLD methods [11].
Quality assessment of the included studies is summarized in Supplementary Table 1. Three studies were considered to be of high quality [9,10,14], and four studies were considered medium quality [11–13,15].
Pooled contamination rates
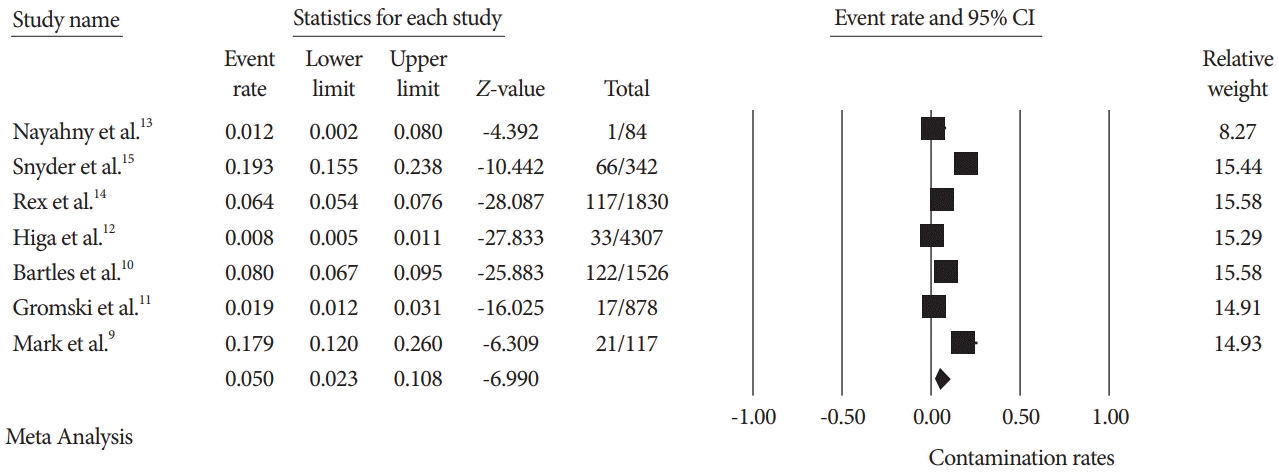
Analysis included a total of seven studies with 9,084 post-ESRT duodenoscope cultures. Pooled analysis of the total weighted contamination rate post-ESRT duodenoscope with both HRO and non-HRO based on the random effects model was 5% (95% CI: 2.3 %–10.8%; I2=97.97%) (Fig. 2).
Secondary outcome
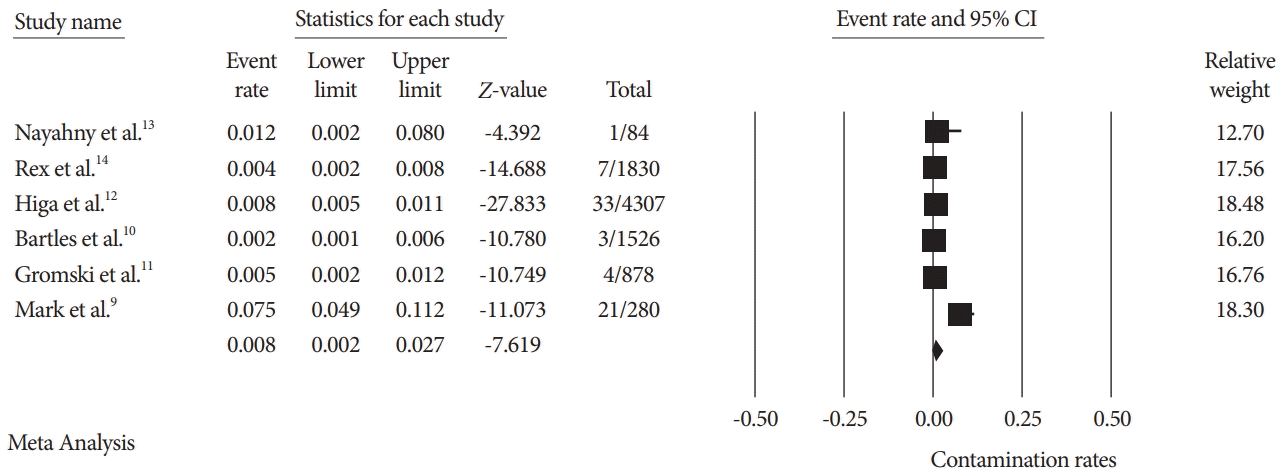
The secondary outcome was to calculate the pooled HRO contamination rates. Snyder et al. [15] did not report any culture positivity for HRO, while all the other studies reported HRO. Among these studies, pooled contamination rates for HRO were 0.8% (95% CI: 0.2%–2.7%, I2=94.96) (Fig. 3).
Heterogeneity and prediction intervals
The I2 statistic provides the ratio of the observed variance that reflects differences in true effect sizes rather than sampling error. I2 was high (97.97%) in the estimation of pooled contamination rates as well as in the estimation of pooled contamination rates of HRO (94.96%).
The prediction interval was calculated to evaluate the dispersion of the effects of the pooled contamination rate. The estimated pooled contamination rate was 0.050 with a 95% CI of 0.023–0.108, and the prediction interval was 0.003–0.499. It is expected that in some 95% of all duodenoscopes comparable to those in the analysis, the true effect size will fall within this prediction interval range. This value is limited due to the small number of studies included in this analysis. Similarly, the prediction interval for HRO contamination was 0.0001 –0.402.
Sensitivity analysis and publication bias
A sensitivity analysis was performed by eliminating one study at a time sequentially to evaluate any possible dominant effect by any single study. This analysis showed that no individual study significantly influenced outcome estimates. The contamination rates with the leave-one-out analysis ranged from 3.9% to 7.4% (Fig. 4). As our analysis contained <10 studies, publication bias was not assessed.
DISCUSSION
The availability of a contaminant-free, patient-ready duodenoscope after disinfection is of utmost importance in preventing duodenoscope-related infections and outbreaks. Contamination of the duodenoscope could reflect possible defects in endoscope cleaning, handling, and storage techniques. Several measures have been taken to mitigate the spread of infection via contaminated duodenoscopes, of which improvement in the disinfection techniques is particularly important [22]. Assessment of contamination rates post-ESRT helps us understand the efficiency of these techniques in providing sterile duodenoscopes, which were reviewed in this study. The current meta-analysis estimated a pooled contamination of 5% in post-ESRT and patient-ready duodenoscopes. While this included both HRO and non-HRO, the pooled contamination rate of HRO alone was 0.8%.
The primary aim of the current study was to examine the pooled contamination rate of duodenoscopes post-ESRT. A prior meta-analysis examining contamination rates after standard HLD reprocessing by Larsen et al. showed a contamination rate of 15.25% in reprocessed duodenoscopes [23]. A subgroup analysis in this study assessing the contamination rate after duodenoscope reprocessing using either dHLD or EtO sterilization reported a contamination rate of 9.2%±0.025%. While the rate of contamination after ESRT was shown to be low at 5% in this study, this remains a significant finding for a process designed to produce a contaminant-free device at completion. The lower contamination rate could be attributed to the inclusion of more studies looking at all FDA-approved ESRT techniques rather than just the EtO and dHLD techniques, such as two studies by Higa et al. and Mark et al. that used culture and quarantine methods [9,12]. Even though they are considered ESRT, the contamination rates here are those after a standard manual clean and HLD process. The implication of patient cross-contamination in these studies should be low because, technically, after each use, a duodenoscope is reprocessed, cultured, and quarantined until no concern about microbial growth is noted. The guidelines on culture and surveillance by the FDA are not truly clear, as they have not defined the frequency of culturing. Two studies with a very rigorous approach of culture and quarantine after each procedure were chosen, with repeat reprocessing before use if any growth was noted. Furthermore, analysis by Higa et al. [12] only reported contamination with HRO; therefore, the rate of contamination with non-HRO in this study is unknown. If these two studies were removed from the analysis, the pooled contamination rate was 6.1% (95% CI: 3.2–11.3, I2=96.05) for both HRO and non-HRO.
The secondary outcome of this study was to calculate the pooled HRO contamination rate. Any growth of HRO is considered clinically significant; hence, looking at duodenoscope contamination with HRO post-ESRT is an important outcome. Studies and interim results from post-market surveillance studies by duodenoscope manufacturers have reported post-standard HLD contamination with HRO to be around 1.9%–5% [1,8], whereas this study showed that post-ESRT duodenoscope contamination with HRO is 0.8%. However, not all studies have reported cultures positive for HRO. Snyder et al. only investigated contamination with multi-drug resistant organisms and not all HRO [15]. Furthermore, this study compared standard HLD, dHLD or standard HLD followed by EtO and did not find any difference in the contamination rate of multi-drug resistant organisms, but this study did not mention HRO contamination. As a result, it was not included in the analysis of HRO contamination rates.
This study had several strengths. To the best of our knowledge, this meta-analysis is the first to assess the impact of various ESRTs on duodenoscope reprocessing. The study included all four ESRTs recommended by the FDA, which included nearly 9,000 duodenoscope cultures. Pooled contamination rates were calculated for both the HRO and non-HRO. Sensitivity analysis was performed by sequentially eliminating a single study at a time to determine if any one study significantly altered the calculated estimates. Other strengths include a thorough and systematic literature search across several databases, in addition to well-defined inclusion and careful exclusion criteria and detailed quality assessment.
This study had several limitations. The number of studies in the current meta-analysis is limited, as only few studies have analyzed the impact of different ESRTs. Heterogeneity in the evaluation of both the primary and secondary outcomes was high. This was possibly because four different techniques were evaluated in this study, with differences in the definition of contamination across various articles. Subgroup analysis to assess the effectiveness of different types of ESRT was not performed owing to their limited number.
Due to their intricate design, elevator mechanism, long working channels, and heat lability, duodenoscopes are exceedingly difficult to disinfect. Other factors that could contribute to duodenoscope cross-contamination include improper manual cleaning or disinfection techniques, human errors, or a combination of these factors. The public health implications associated with patient cross-contamination during ERCP are significant. With different ESRTs recommended, the adoptability of any single method by an institution depends on the cost, local expertise, and availability of resources. For example, EtO sterilization is expensive and is not universally available. Culture and quarantine are time consuming and expensive. In addition to improving disinfection techniques, the FDA has also recommended transitioning to innovative duodenoscope designs that can be easily reprocessed or disposed. FDA has cleared two fully disposable duodenoscopes, three disposable duodenoscope endcaps, and one disposable elevator duodenoscope [24]. A trend toward transitioning to partially or completely disposable duodenoscopes has begun. While some studies have shown benefits in preventing cross-contamination with disposable components, further longer-term studies are needed [25]. Fully disposable duodenoscopes have the advantage of eliminating the need for reprocessing and potentially eradicating all cross-contamination risks. Studies have shown equivalent performance of disposable duodenoscopes to conventional ones; however, further studies on safety, efficacy, cost, and environmental impacts are needed [26,27].
In conclusion, while the contamination rates and disinfection process may have improved with ESRT, a contamination rate of 5% is still significant. Further studies are warranted to evaluate the efficacy of each technique and to recommend standardized, economically reasonable, easily available, and safe disinfection/sterilization techniques. A considerable contamination rate despite enhanced techniques warrants innovations in duodenoscope design and disposable duodenoscopes, which are also important means to help mitigate cross-contamination and outbreaks.
Supplementary Material
Supplementary Material 1.
Actual Search Strategies
Supplementary Table 1.
Quality Assessment of the Included Studies
Notes
Conflicts of Interest: Richard A Kozarek is a Research support for Boston Scientific and NIH. Andrew Ross is a consultant for Boston Scientific. The other authors have no potential conflicts of interest.
Funding
None.
Author Contributions
Conceptualization : Shivanand Bomman, Rajesh Krishnamoorthi
Data curation: SB, Navroop Nagra, Shruti Chandra
Formal analysis: SB, Munish Ashat, NN, Mahendran Jayaraj, RK
Investigation: SB, NN, MJ, SC
Methodology: SB, RK
Supervision: Richard A Kozarek, Andrew Ross
Validation: SB, MA, NN, MJ, SC, RAK, AR, RK
Visualization: SB, NN
Writing-original draft: SB, RK
Writing-review&editing: SB, MA, NN, MJ, SC, RAK, AR, RK