Endoscopic Treatment of Intussusception due to Intestinal Tuberculosis
Article information
Abstract
Traditionally, adult intussusception has required a bowel resection because of the malignancy risk. A patient with anorexia, weight loss, and abdominal pain visited our clinic. A physical exam and imaging study revealed no acute peritoneal signs. A colonoscopy for biopsy and bowel reduction was attempted. The tissue sample was consistent with intestinal tuberculosis. We report intestinal tuberculosis complicating intussusception which was treated without surgical intervention.
INTRODUCTION
Tuberculosis can affect any part of the gastrointestinal tract [1]. The symptoms of intestinal tuberculosis are non-specific. Obstruction, perforation, or ischemia can occur as the disease progresses [2].
Adult intussusception is rare. Pediatric intussusception is far more common than the adult type. Between 1% and 5% of intestinal obstructions in adults are caused by intussusception [3,4]. An identifiable lead lesion is found in 70%–90% of intussusception cases [5,6].
CASE REPORT
A 64-year-old Korean man with weight loss, anorexia, and abdominal pain was admitted.
The patient’s blood pressure was 109/69 mm Hg, his body temperature was 38.1°C, his heart rate was 88 beats per minute, and his respiratory rate was 20 breaths per minute. On physical examination, coarse crackles were audible in the right lung. A soft mass was palpable in the right lower abdomen. The patient did not have neurologic impairment or related medical history.
The patient’s white blood cell count was 11.6×109/L, his hemoglobin was 13.5 g/dL, his platelet count was 396×109/L, and his C-reactive protein was 12.3 mg/dL. Tumor markers were within the normal range. A sputum acid-fast bacilli stain, sputum culture, and polymerase chain reaction were positive for Mycobacterium tuberculosis.
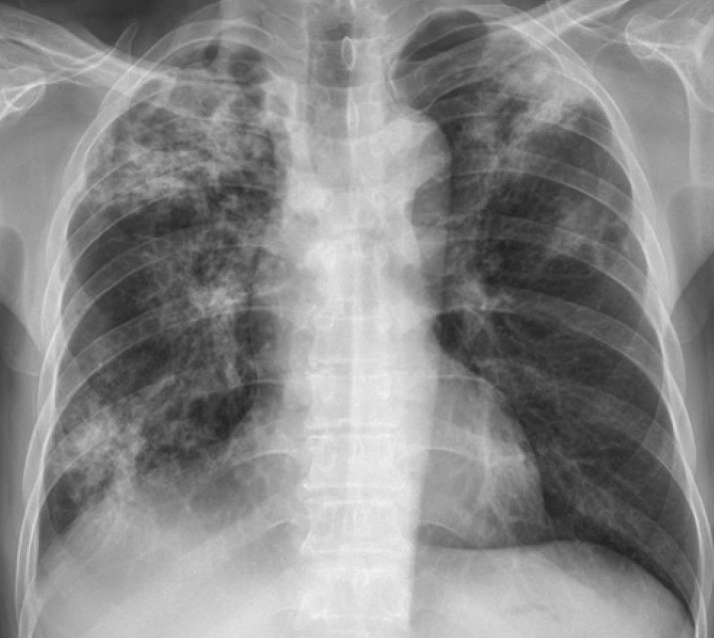
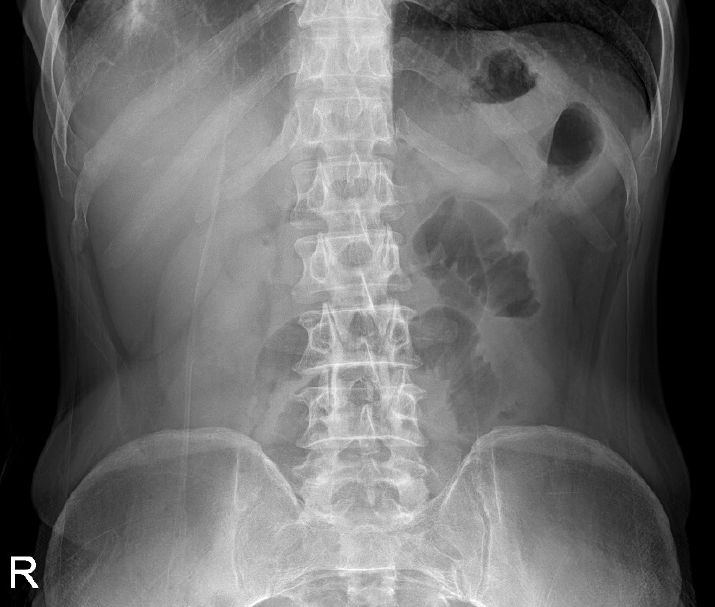
Plain chest X-ray showed consolidations with cavities (Fig. 1). Simple abdomen X-ray showed no significant obstruction (Fig. 2).
On a contrast-enhanced abdominal computed tomography (CT) image (Fig. 3), the bowel wall was overlapped in a donut shape, and multiple mesenteric lymph nodes were enlarged.

Abdominal computed tomography (CT) showing the target lesion with alternating densities, which were the intussusceptum (inner layer) and intussuscepien (outer layer) (arrow).
The patient was without acute peritoneal signs and not in urgent clinical condition. A colonoscopy was scheduled to obtain a biopsy that could rule out malignancy. Bowel preparation using the usual laxative amount was accomplished without abdominal pain or complications. There was a report that bowel preparation should be performed with caution because it may accelerate intussusception [7]. However, there was also a report that a colonoscopy had been used to diagnose the exact level of intussusception and reduce intussusception by air infusion [8].
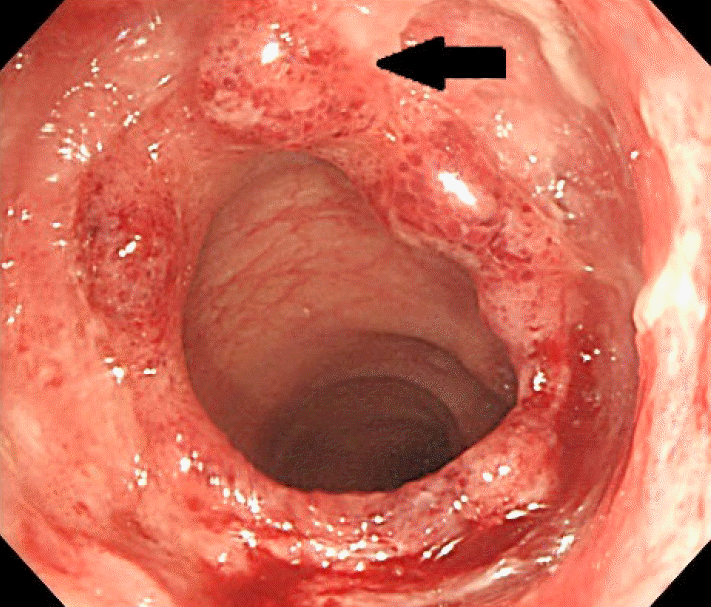
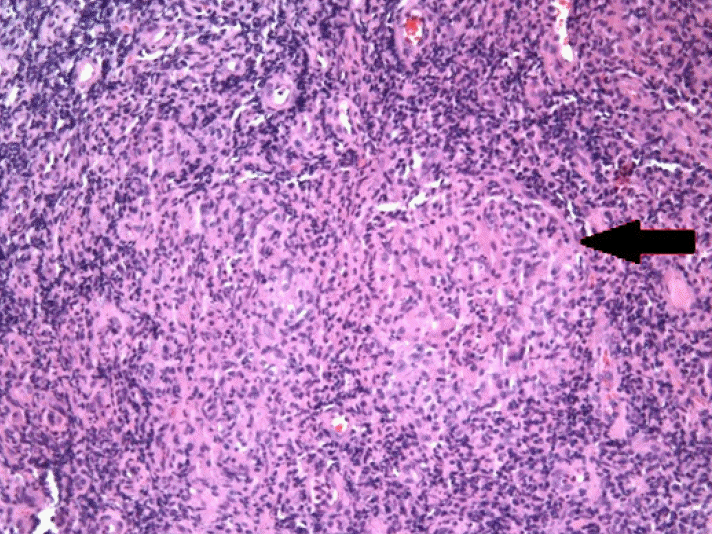
An asymmetric hypertrophied mass on the ileum was noted in the endoscopy (Fig. 4). Manual reduction of the intussusception was achieved using air infusion. No image was taken before the intussusception reduction. The biopsy results indicated an ulcerative, necrotic, and inflammatory lesion with a granuloma, which is consistent with intestinal tuberculosis (Fig. 5). There was not a high degree of dysplastic or tumor cells.
A round of standard anti-tuberculosis medication was administered and the patient’s symptoms were relieved.
DISCUSSION
Intussusception is a serious condition in which a segment of the intestine slides into an adjacent part of the intestine [9]. Most cases of adult intussusception are the result of an underlying clinical condition. Adult intussusception presents without specific symptoms. Benign masses and adhesion are the most common causes of small bowel intussusception, causing about 90% of cases [10,11]. Adenocarcinoma is the most common cause of large bowel intussusception [12].
Abdominal CT is a useful tool in diagnosing intussusception [13]. The typical CT finding is an inhomogeneous target or sausage-shaped mass. The mesenteric vessels and fat can be seen between the bowel walls [12]. Colonoscopy is a useful tool for diagnosing adult intussusception [4,14,15]. A colonoscopy can confirm and localize the intussusception while also revealing the underlying lead point lesion. Polypectomy of the lead point is not recommended because of the high risk of perforation and necrosis of the bowel.
The conventional management method is a surgical resection using an oncologic technique because the underlying medical conditions often involve malignancy. Preoperative reduction of intussusceptions is not recommended because it can cause tumor cell seeding and weaken the mucosal wall. The prognosis is generally favorable after surgery. Metastases in the small intestine result in the poorest prognosis in adult intussusception.
Intestinal tuberculosis is caused by Mycobacterium tuberculosis or atypical mycobacterium, the latter being associated with acquired immune deficiency syndrome (AIDS) [16]. The postulated mechanisms by which the tuberculosis bacilli reach the gastrointestinal tract are hematogenous spread, ingestion of bacilli in sputum, and through lymph channels from infected nodes [1]. The most frequent site of involvement is the ileocecal junction.
Diagnosis is usually confirmed by radiologic, endoscopic, and histologic modalities [1]. Asymmetric thickening of the colonic wall and enlarged necrotic lymph nodes were highly suggestive CT findings [17]. Using an endoscopic biopsy, diagnosis is possible if the acid-fast bacillus (AFB) stain or caseating granuloma is positive. Treatment of intestinal tuberculosis is the same as that of pulmonary tuberculosis, unless there are acute abdominal signs [18].
Adult intussusception caused by intestinal tuberculosis was reported by Nakamura et al. [9] and Kang et al. [19]. In both cases, segmental resection of the bowel was performed. This case had a different therapeutic approach as endoscopic reduction was performed. It is suggested that a more conservative treatment is plausible unless acute abdomen or high malignancy risk is present.
The traditional treatment plan for adult intussusceptions has been changing. Kim et al. suggested that, if the length of the intussusception is shorter than 3.5 cm and there is no leukocytosis and no obstruction, manual reduction by endoscopy can be safely attempted [20]. We report a case of intussusception due to intestinal tuberculosis and suggest a more conservative approach to treating adult intussusceptions to avoid unnecessary bowel resections.
Notes
Conflicts of Interest: The authors have no financial conflicts of interest.