Feasibility of single-session endoscopic ultrasound-guided liver biopsy and endoscopic retrograde cholangiopancreatography in liver transplant recipients with abnormal liver function tests
Article information
The two most common post-liver transplant (LT) complications include T-cell mediated rejection (TCMR) and biliary pathologies, such as strictures, leaks, and stones/casts.1 Both manifest with abnormal liver function tests (LFTs) with various patterns, including cholestatic, hepatocellular, or mixed.1 Standard work-up entails a detailed history and physical examination, laboratory tests, and imaging of the liver/biliary tree to identify patients requiring a liver biopsy for TCMR or an endoscopic retrograde cholangiopancreatography (ERCP) for suspected biliary pathology. However, the yield of biliary imaging in the post-LT setting remains low, with ultrasound having a sensitivity of 29% and specificity of 69%, whereas magnetic resonance imaging having a sensitivity of 78% and specificity of 56%.2
Liver biopsies have traditionally been performed using a transjugular or percutaneous route. Recently, endoscopic ultrasound (EUS)-guided liver biopsy (EUS-LB) has emerged as a safe and effective method for obtaining liver histology.3,4 A meta-analysis of nine studies and 437 patients demonstrated a histologic diagnosis rate of 93.9% (95% confidence interval, 84.9%–97.7%) and an adverse event rate of 2.3% (95% confidence interval, 1.1%–4.8%).4 EUS-LB typically requires a slightly smaller (19 G) needle than the standard 16 or 18 G needle used in a transjugular or percutaneous biopsy. However, EUS allows sampling of both the right and left lobes of the liver, which can yield a greater specimen length and number of complete portal tracts than percutaneous biopsy.3
In cases of non-diagnostic patterns of abnormal LFTs and inconclusive imaging studies, clinicians often face the conundrum of choosing between appropriate tests and the sequence (liver biopsy or ERCP) with which tests should be performed. Additionally, patients may simultaneously have more than one condition i.e., TCMR and anastomotic stricture, which further adds to the diagnostic dilemma. Delay in treatment can further complicate this challenging situation. Therefore, we studied the feasibility of single-session EUS-LB and ERCP in post-LT patients with abnormal LFTs which lack a clear etiology, defined as those patients for whom the standard work-up did not lead to a clear diagnosis.
This single-center retrospective study examined post-LT patients who underwent concomitant EUS-LB and ERCP between January 2021 and July 2021. Demographic data, laboratory and diagnostic results, management, and adverse events were recorded. The R factor was calculated as the serum alanine aminotransferase/upper limit of normal divided by the serum alkaline phosphatase/upper limit of normal. The study was approved by the Ohio State University Institutional Review Board (No: 2021H0212).
All adult post-LT patients from January 2021 to July 2021 who underwent LT within one year and presented with abnormal LFTs and non-diagnostic imaging studies were referred for concomitant EUS-LB and ERCP. The decision to perform single-session EUS-guided LB and ERCP was jointly made by the transplant hepatology and surgery teams, and only patients who underwent both procedures in a single session were included. Patients who underwent EUS-LB or ERCP in separate sessions were excluded.
All procedures were performed by an experienced therapeutic endoscopist. In our approach, EUS-LB was performed first, followed by ERCP, with patients under general anesthesia. EUS-LB was performed with a linear echoendoscope using a 19 G fine needle biopsy needle (Acquire; Boston Scientific) via the wet suction technique.5 The needle was primed with heparin and a 20-mL suction syringe was used. Left lobe biopsy was performed using a transgastric route with 3 to 7 actuations in a fanning method during a single pass. Similarly, a right lobe biopsy was performed using a transduodenal route. Color Doppler ultrasound was utilized to avoid any blood vessels. After each pass (two passes), specimens were placed in separate containers with 10% formalin and were reviewed by the pathology department. ERCP was subsequently performed in the standard fashion for biliary evaluation. Endotherapies such as biliary sphincterotomy, balloon dilation of strictures, stone/cast removal, and/or stent insertion were performed based on the cholangiogram findings at the discretion of the endoscopist. All patients were observed for a short period in the post-anesthesia care unit before being discharged if they were outpatients or sent to their hospital beds if they were inpatients.
The primary outcome was a technical success, defined as the successful completion of both procedures in a single session. The secondary outcomes included EUS-LB tissue adequacy and adverse events. Our expert liver pathologists determined tissue adequacy as containing ≥11 complete portal tracts. Adverse events were defined and categorized as per the American Society for Gastrointestinal Endoscopy guidelines.6,7 Descriptive statistics were used to depict outcomes in terms of mean with standard deviation or proportion (n, %).
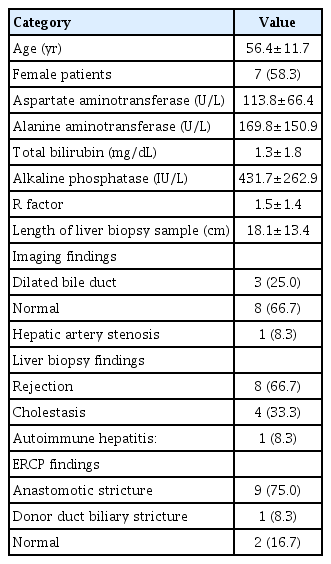
During the 6-month study period, 70 LTs were performed. Of these patients, 18 underwent either ERCP or liver biopsy, while 12 underwent concomitant EUS-LB and ERCP for the work-up of abnormal LFTs (Table 1). All 12 patients underwent cadaveric LTs. The mean alanine aminotransferase was 169.8±150.9 U/L, and the mean alkaline phosphatase was 431.7±262.9 IU/L with a mean R factor of 1.5±1.4.
The mean procedure time was 66.8±30.1 minutes (mean of 10.1 minutes for EUS-LB itself), and technical success was achieved in 100% of cases. As per pathologist interpretation, the mean total liver specimen length (sum of all cores from left and right lobes) was 18.1±13.4 cm and 100% of liver samples had tissue adequacy. TCMR was found in the biopsy of 66.7% (n=8) of the patients and anastomotic strictures in 75.0% (n=9) of the ERCPs (Table 1). Seven (58.3%) patients had concomitant diagnoses of TCMR and anastomotic strictures (Fig. 1). There were no occurrences of 30-day adverse events.
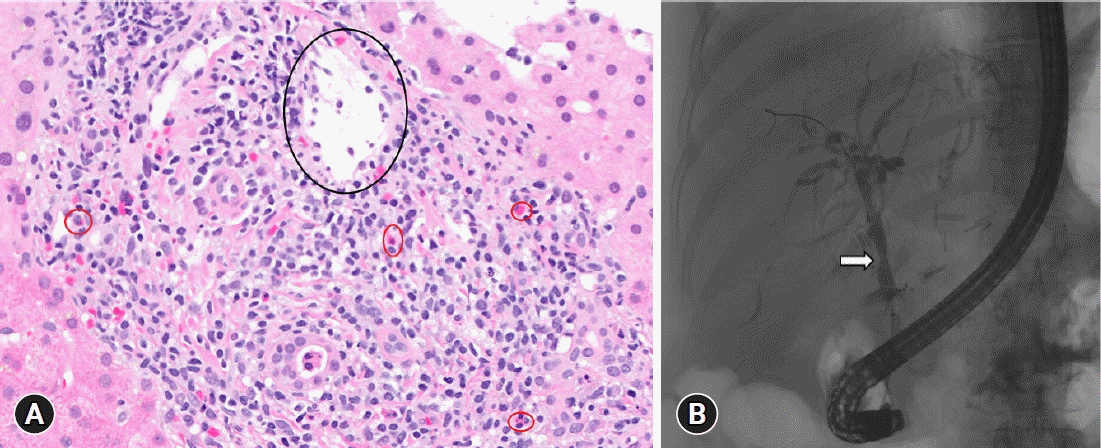
Pathology image of a portal tract demonstrating T-cell mediated rejection with a black circle indicating portal vein endotheliitis and red circles marking eosinophils (A, hematoxylin and eosin stain, ×400) and a cholangiogram indicating an anastomotic stricture (B, arrow) in a patient with concomitant rejection and anastomotic stricture.
The work-up of abnormal LFTs in the post-LT setting remains challenging, and early diagnosis can have significant ramifications. Diagnostic algorithms are not very accurate in guiding physicians to choose between liver biopsy or ERCP in differentiating the two most common post-LT complications. Furthermore, there may be a delay in management, increased costs, and the need for resources when starting with one intervention and then switching to another at a different time point. With the introduction of EUS-LB, we proposed a paradigm shift in the management of a select group of post-LT patients with abnormal LFTs using single-session EUS-LB and ERCP.
In this pilot study, we demonstrated the feasibility of combining the two interventions successfully in a single session to obtain one or two composite diagnoses. Strikingly, more than 50% of the patients had two concomitant diagnoses (TCMR and anastomotic stricture). This led to a change in management and highlighted the possibility of multiple complications in transplant patients with abnormal LFTs. Although limited by the small sample size of patients in our series, no adverse events occurred with either intervention. While ERCP is typically reserved for therapeutic indications, post-transplant biliary evaluation remains one of its few diagnostic indications. The low post-ERCP pancreatitis rate observed in this population coupled with the low adverse event rate of EUS-LB suggests that the combination of the two offers an acceptable safety profile.4,8
In addition to EUS-LB, the recent development of EUS-guided portal pressure gradient measurement offers a potential avenue for further streamlining the work-up of post-LT patients with suspected portal hypertension and fibrosis.9 Pilot studies have demonstrated an excellent correlation of EUS-guided measurements with the standard transjugular approach. A recent study demonstrated the feasibility of performing both EUS-guided portal pressure gradient measurement and EUS-LB in a single procedure.9,10
In conclusion, this single-session approach combining EUS-LB and ERCP was found to be feasible and safe in a pilot cohort of post-LT patients with abnormal LFTs. As we would not recommend this approach in all post-LT patients with abnormal LFTs, further prospective multicenter studies are needed to evaluate its use in patients with mixed patterns of LFT elevation and/or an unclear etiology of injury. Moreover, its cost-effectiveness must be evaluated in the context of post-LT management.
Notes
Conflicts of Interest
The authors have no potential conflicts of interest.
Funding
None.
Author Contributions
Conceptualization: SH, SJ, KM; Formal analysis: SH, SJ, KM; Investigation: all authors; Methodology: SH, SJ, KM; Writing–original draft: SH, SJ, KM; Writing–review & editing: all authors.