INTRODUCTION
Midgut malrotation is a potential cause of bowel obstruction in children. A symptomatic association between a malrotation and a congenital duodenal web is rare and few cases have been reported in the literature. The true incidence of malrotation is not fully known; however, it is reported as approximately 1 in 500 live births [1,2]. The incidence of duodenal web as a cause of intestinal obstruction is reported to be between 1:10,000 to 1:40,000 [3,4]. There is a high incidence (approximately 50%) of associated anomalies in patients with intrinsic duodenal obstruction, but malrotation is reported to occur in only in 19.7% of cases [4]. We present our experience with four patients at two centers (Siena and Ancona) and a review of the literature.
CASE REPORTS
Case 1
A 2-year-old girl was transferred to our clinic with a history of nonbilious vomiting since 2 months of age and loss of weight (8.8 kg). On admission, the patientŌĆÖs vital signs were normal. On physical examination, her abdomen was soft and nontender with no peritoneal signs. Her anus was normal and an abdominal ultrasound was normal. An upper gastrointestinal contrast study revealed a duodenal obstruction. Laparotomy was performed and a distended duodenum with the cecum and appendix at the left upper quadrant fixed by LaddŌĆÖs bands was found. LaddŌĆÖs procedure was performed and the appendix was removed. The patientŌĆÖs postoperative course was normal.
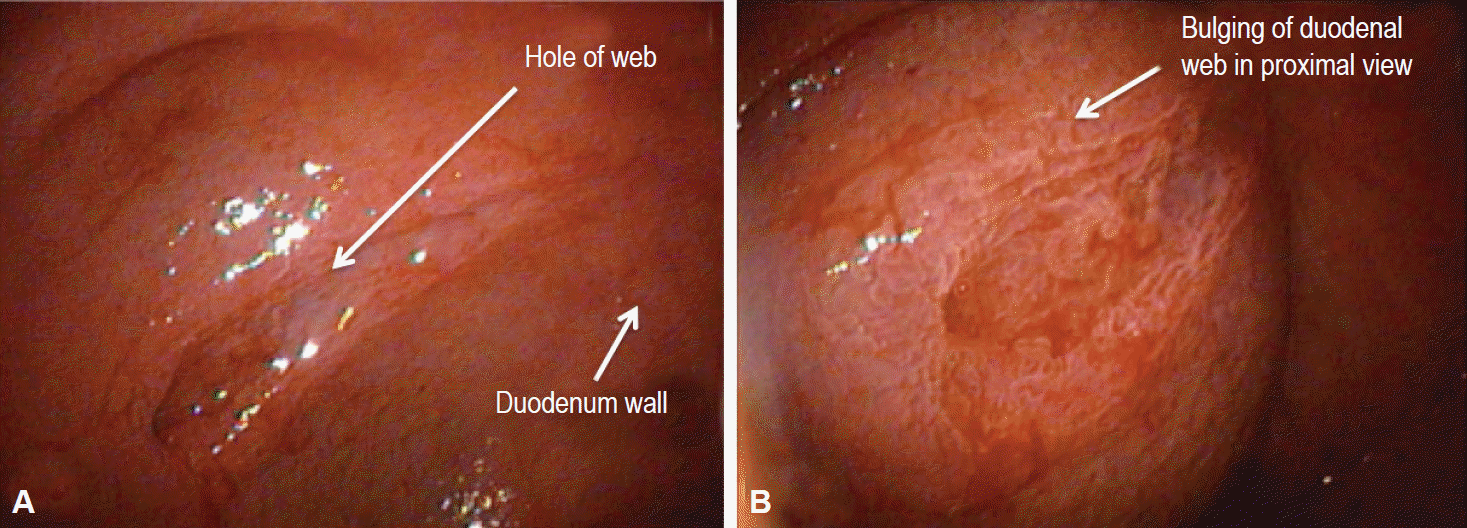
Two months after surgery, she was hospitalized for persistent diarrhea and nonbilious vomiting. An upper gastrointestinal contrast study was performed and it showed delayed gastroduodenal emptying. Esophagogastroduodenoscopy revealed a duodenal web with a small central defect that we attempted to manage endoscopically (endoscopic resection) with no success (Fig. 1). Parental nutrition (PN) was started and a second laparotomy was performed. The duodenum was opened and the antimesenteric border of the duodenal web was excised; a side-to-side duodenoduodenostomy was completed. The patient tolerated full oral feeding on day 6 after surgery. The PN was withdrawn on the postoperative day 10 and she was discharged on day 11. At last follow-up, 4 weeks after discharge, the patient had gained 900 g and she fed without problems.
Case 2
A 5-day-old boy, delivered by caesarian for fetal bradycardia, was evaluated for nonbilious vomiting since birth and loss of 10% of his birth weight (2,980 g). Normal meconium passing was noted. Malrotation was suspected based on an upper gastrointestinal X-ray analysis. An echocardiogram analysis ruled out any congenital cardiac anomalies. The patient underwent laparotomy that showed a middle distended duodenum with the cecum and appendix at the left upper quadrant fixed by LaddŌĆÖs bands. LaddŌĆÖs procedure and an appendectomy were performed. The absence of bile in the nasogastric tube and failure to pass a nasogastric tube through the duodenum led us to perform a duodenotomy. Opening of the duodenum showed a large duodenal web with a blind pouch. Distal to the web, the duodenum was normal. The duodenal web was resected and the duodenum was closed. The patient was transferred to the neonatal intensive care unit. The nasogastric tube was left in place for 5 days and PN was provided. An upper gastrointestinal exam was performed on postoperative day 8 and it showed no leakage. Oral feeding was started and it was tolerated well. He was discharged home on postoperative day 28 with a weight of 3,620 g. Two weeks post discharge the patient was breastfeeding normally with an increase in weight to 4,020 g.
Case 3
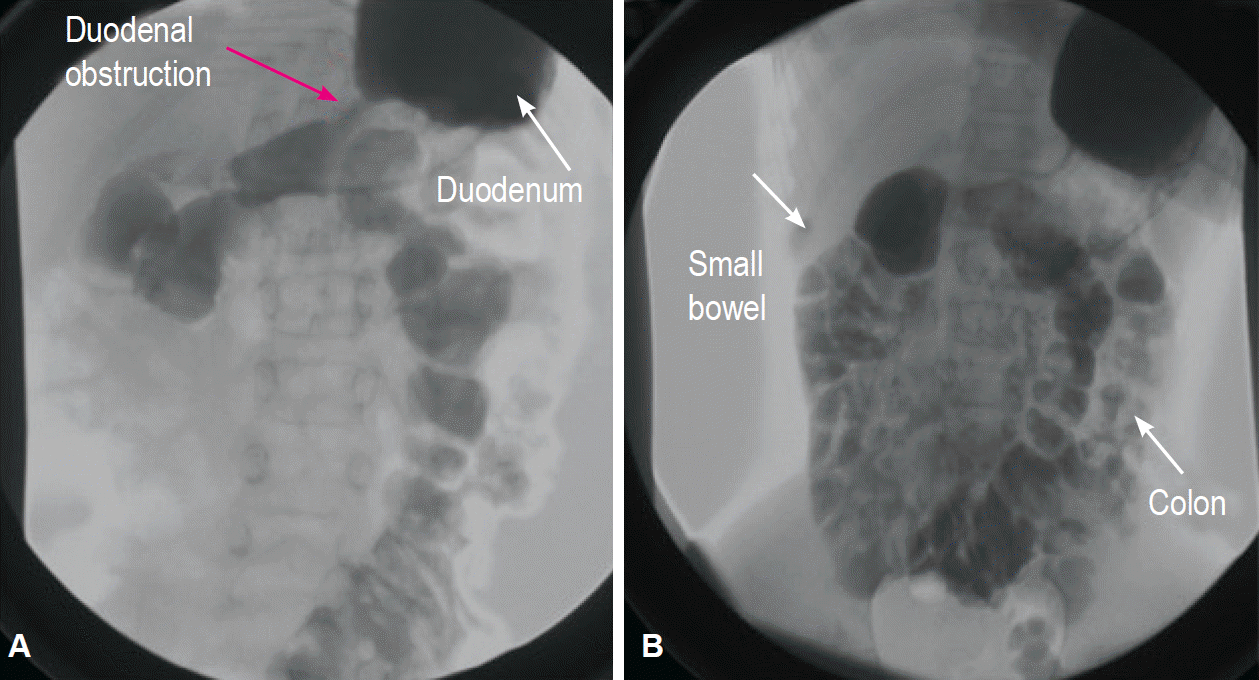
A 10-year-old girl came to our outpatient clinic for persistent nonbilious vomiting since birth. She had trisomy 21. She had been operated on for malrotation at 8 months (ValdoniŌĆÖs procedure) and for duodenal stenosis at 9 months (duodenotomy and resection of a congenital web). She underwent laparoscopic adhesiolysis for bowel obstruction at age 5. An upper gastrointestinal contrast study showed a duodenal stenosis with delayed emptying of the 2nd duodenal portion with all of the small bowel in the right quadrant and the colon in the left quadrant due to the previous ValdoniŌĆÖs procedure (Fig. 2). Esophagogastroduodenoscopy was performed and it confirmed the persistence of the duodenal web. We planned a laparotomy and performed a side-to-side jejunal duodenum anastomosis. After 24 hours in pediatric intensive care, the patient was transferred to our ward, where oral feeding was started with a gradual increase day by day. She was discharged on postoperative day 10, with complete tolerance of the oral diet. At outpatient follow-up, 1 month after discharge, she took food and drinks orally without difficulty and she did not experience any vomiting.
Case 4
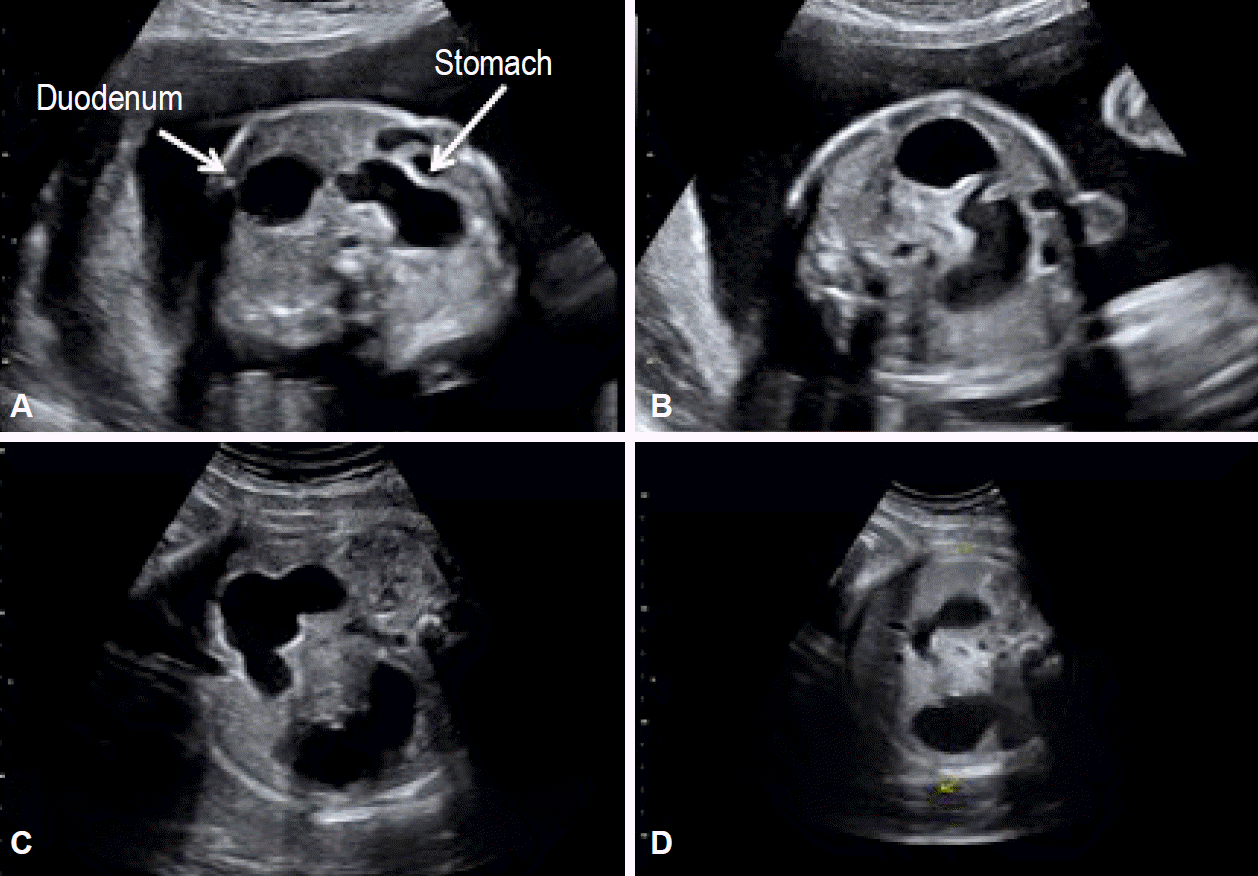
A 1-day-old boy was evaluated for prenatal diagnosis of a double bubble (Fig. 3). After birth, radiography showed an enlarged stomach and duodenum and air in the distal bowel. An upper gastrointestinal series revealed an incomplete duodenal obstruction. Surgery confirmed the presence of a congenital duodenal web and revealed the presence of malrotation. An esophagogastroduodenoscopy was performed and the procedure confirmed the persistence of the duodenal web. We performed a LaddŌĆÖs procedure and duodenotomy with resection of the web. His postoperative course was normal. The nasogastric tube was left in place for 5 days and PN was administered. An upper gastrointestinal exam was performed on postoperative day 7 and it showed no leakage. Oral feeding was started and it was tolerated well. He was discharged home on postoperative day 19. He will attend the outpatient clinic in a month.
DISCUSSION
A symptomatic malrotation usually presents during infancy or during the neonatal period; however, many cases are reported at older ages [4]. An early diagnosis is important because of the high risk of a life-threatening midgut volvulus [4]. The most common presentation of malrotation is bilious vomiting due to duodenal obstruction from intermittent midgut volvulus rather than compression by LaddŌĆÖs bands or kinking of the duodenum [4]. However, in some patients, malrotation is discovered incidentally during radiographic studies or during laparotomy performed for other indications [1,2,5,6].
Congenital duodenal obstruction is a frequent cause of congenital intestinal obstruction in the newborn, occurring in 1 per 5,000 to 10,000 live births, affecting boys more commonly than girls [4]. Duodenal obstruction results from either intrinsic or extrinsic lesions. More than 50% of patients with duodenal atresia or duodenal stenosis have associated congenital anomalies, especially Down syndrome, which is present in around 30% of duodenal obstruction patients [4]. The associated malformations in order of frequency are Down syndrome, annular pancreas, congenital heart disease, malrotation, esophageal atresia, urinary tract malformation, anorectal anomalies, other bowel atresias, vertebral anomalies, and musculoskeletal anomalies. These associated malformations have an impact on the morbidity and mortality of these patients [3,4,7].
The intent of this report was to focus on the uncommon but possible association between intestinal malrotation and intrinsic duodenal obstruction (19.7% of cases) [5]. Our review of the literature is summarized in Table 1 [8-20]. Through this brief review, it is clear that since 1950 an association between duodenal malformation and intestinal malrotation has been noted. However, it is evident from the review that this association is uncommon highlighting the difficulty associated with preoperative diagnosis. There are currently 94 reported cases of duodenal malformation associated with malrotation. However, only 15 of 94 (16%) include patients with malrotation and duodenal webbing. The four cases of the present study (Table 2) add to the literature and further support the idea that during the surgical treatment of a patient with duodenal obstruction, it is necessary to exclude the co-occurrence of malrotation and intrinsic duodenal pathology to avoid having to perform two surgeries in a short period.
We performed a retrospective analysis of our series. The first case affirms that the clinical and imaging picture of the patient was discordant with the initial diagnosis. The baby was referred to us with nonbilious vomiting and failure to thrive since birth. An initial suspicion of a pyloric stenosis was unlikely based on the history and it was ruled out based on ultrasound and laparotomy observations. During the first laparotomy, intestinal malrotation without volvulus was found; however, this could not explain the clinical findings of nonbilious vomiting and metabolic alkalosis. A classic malrotation ŌĆ£usuallyŌĆØ presents with bilious vomiting because the obstruction is under VaterŌĆÖs papilla. The absence of bilious vomiting should have alerted us to the possibility that a second pathology at the level of the gastric antrum or proximal duodenum was present, which was confirmed during the second surgery. An esophagogastroduodenoscopy could have aided the diagnosis.
The second case showed the correct management of a child with nonbilious vomiting and intraoperative confirmation of LaddŌĆÖs band. In the presence of malrotation, on the basis of the absence of bile in the nasogastric tube and the impossibility of passing a nasogastric tube through the duodenum, we explored the duodenum and found the duodenal web. The third case, as in the first, demonstrated wrong initial management because the patient underwent two different surgeries. The last case was a simple paradigmatic case because the presence of the duodenal web and malrotation was an incidental finding during surgery. Esophagogastroduodenoscopy established the correct diagnosis.
In conclusion, we suggest that an incidental finding should not distract surgeons from finding the underlying pathology. Indeed, even if some associations are described as rare and uncommon, they could occur in a patient. Nonbilious vomiting in a child must prompt the surgeon to consider a duodenal pathology even in the presence of malrotation. A preoperative esophagogastroduodenoscopy, when it is possible, is a good approach for surgeons to confirm the presence of a duodenal web. The alternative, duodenal exploration is imperative to exclude the involvement of a duodenum web as the cause of vomiting.