INTRODUCTION
Recent technical developments have resulted in the remarkable development of novel endoscopic devices and accessories, even though most are applied using an over-the-scope or over-the-guidewire method rather than a through-the-scope method. In particular, the use of endoscopic treatment with novel devices and methods allows for targeting of not only neoplastic lesions, but also chronic disorders, such as gastroesophageal reflux disease (GERD) and obesity. In both conditions, there is a treatment gap between medical and surgical therapy and an unmet need for less invasive treatment. To bridge this gap, endoscopic management has been the focus of research.
GASTROESOPHAGEAL REFLUX DISEASE
GERD is a common disorder, affecting 20% of the adult population in the US every week [1]. The prevalence of GERD has been reported to be 18.1%ŌĆō7.8% in North America, 8.8%ŌĆō25.9% in Europe, and 4.6%ŌĆō10.7% in Korea [2-4]. The true incidence of GERD may be higher since over-the-counter medications, such as antacids and proton pump inhibitors (PPIs), are available in many countries. Currently, medical, endoscopic, and surgical treatment are used for patients with GERD. Although PPIs have been the mainstay of medical management of GERD, there are patients who do not respond to or require chronic PPI use. The potential adverse effects of the chronic use of PPIs are also of concern. These adverse effects include enteric infections including Clostridium difficile, increased susceptibility to pneumonia, hypergastrinemia, hypomagnesemia, and higher incidence of chronic kidney disease in susceptible populations [5,6]. In the late 1990s, a series of endoscopic treatments for GERD were introduced, but have failed to show long-term efficacy. These treatments included implantation and injection devices (Enteryx, Gatekeeper) and tissue apposing devices (EndoCinch and NDO plicator). Nonetheless, there has been an increased interest among patients and medical professionals in minimally invasive endoscopic intervention as an alternative to surgical treatment. Endoscopic procedure can be done in out-patient basis, and is expected to avoid side effects of laparoscopic NissenŌĆÖs fundoplication, such as bloating and dysphagia [7,8]. Four endoscopic treatment modalities are clinically available presently: radiofrequency (RF) treatment with the Stretta device, transoral incisionless fundoplication (TIF) with either the EsophyX device or Medigus ultrasonic surgical endostapler (MUSE), and anti-reflux mucosectomy (ARMS). In this review, I excluded MUSE which requires a novel endoscopic system and ARMS which use conventional endoscopic accessories for the procedure.
Radiofrequency ablation
The Stretta procedure, a RF application for the lower esophageal sphincter (LES), was introduced approximately 15 years ago [9]. Since the initial introduction of the Stretta RF system, several minor modifications have been conducted that have facilitated the ease of use and proper application of the technique. The Stretta procedure appears to result in thickening of the LES, decreased transient LES relaxation rate, and reduced esophageal acid exposure. Possible adverse events (AEs), such as esophageal stricture or neurolysis in the distal esophagus, have not been reported over time [10-12]. The Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has indicated Stretta as an recommended therapeutic option for patients with GERD, who are over age 18, have suffered symptoms of heartburn and/or regurgitation for at least 6 months, who have had complete or partial response to antisecretory drug medication, and who have refused surgical management [13].
The Stretta system (Mederi Therapeutics, Greenwich, CT, USA) consists of a four-channel RF generator and single-use RF energy catheters. This system delivers pure sine-wave energy (465 kHz, 2 to 5 W per channel). Each needle tip incorporates a thermocouple that automatically adjusts the power output to a desired target temperature in the muscle layer. Automatic thermoregulation maintains the temperature of the electrode below 100Ōäā to minimize neighboring tissue damage due to vaporization and high impedance values. Power delivery stops if mucosal temperature exceeds 47Ōäā [9]. RF energy is applied to four points located 1 cm proximal to the Z line first. Next, change the direction of the electrodes about 45┬░ degree, and RF energy is applied to four more points at the same level delivering RF energy to a total of eight points at the same level. This procedure is repeated at three more levels at intervals of 0.5 cm (Fig. 1) [14]. The potential action mechanism of RF delivery appears to be related with smooth muscle hypertrophy at the cellular level in an animal model which includes redistribution of the interstitial cells of Cajal and a change in the muscle fiber to connective tissue ratio (increase in collagen 1 and decrease in collagen 3 [15].
Transoral incisionless fundoplication
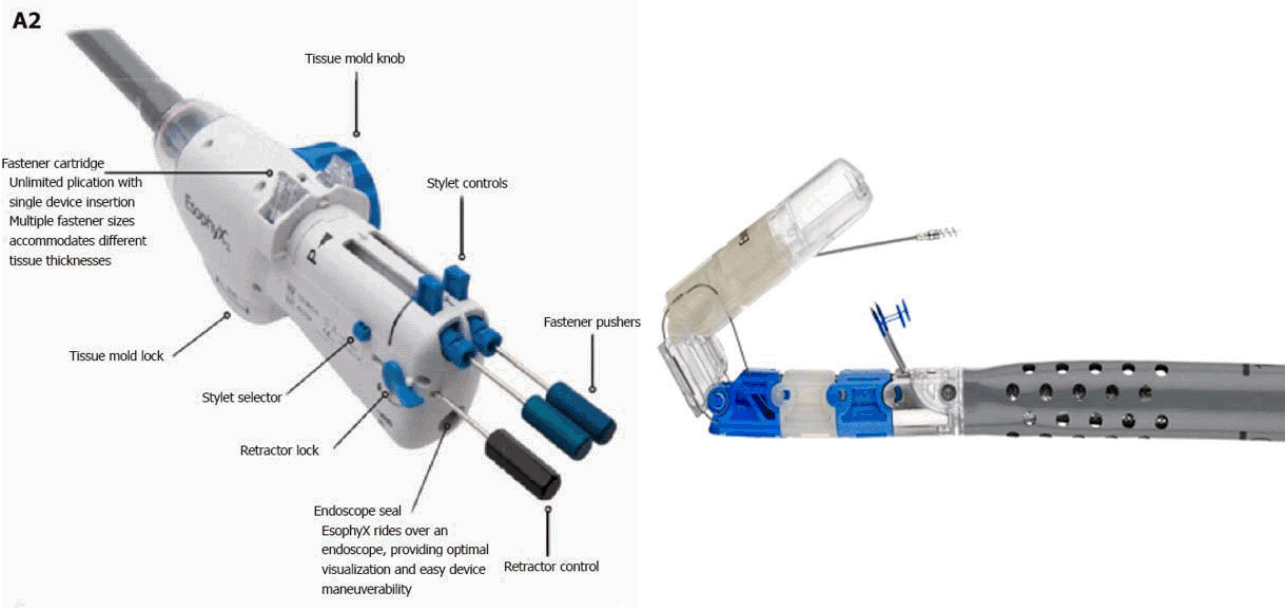
The TIF is a minimally invasive therapeutic procedure for GERD that is done transorally from the inside of patientŌĆÖs stomach without incisions. This procedure delivers patient outcomes similar to those of conventional anti-reflux surgery (ARS) procedures, but is less invasive. The TIF procedure reconstructs the gastroesophageal valve through a partial fundoplication and helps to restore the dynamics of the angle of His as the anti-reflux barrier. EsophyX device (EndoGastric Solutions, Inc., Redmond, WA, USA) is consisted with is consisted with: (1) a handle; (2) an 18-mm diameter frame that includes operative channels through which a frontview 9-mm diameter endoscope can be inserted; (3) the invaginator, provided by side holes on the distal part of the chassis, to which external suction can be applied; (4) the tissue mold, which can be brought into retroflection and pushes tissue against the shaft of the device; (5) a helical retractor, which is advanced into the tissue so the tissue between the tissue mold and the shaft can be retracted; (6) two stylets, which pass through the plicated tissue and the tissue mold, and H-shaped polypropylene fasteners which maintain tissue compression throughout healing process can be deployed over them; and (7) a cartridge containing 20 fasteners. Recently updated instrument, the EsophyX Z device has fastener deployment to reduce control complexity. Under the direct visualization of the endoscope, the device is positioned within the LES muscle and sturdy anti-reflux valve can be created. The procedure is performed under general anesthesia (Fig. 2) [16].
OBESITY
Obesity represents a major health issue around the world. This multifactorial chronic disease has a growing prevalence and has reached epidemic proportions over the previous few decades [17]. According to recent survey results, more than half (53.8%) of the adult population in Organization for Economic Cooperation and Development (OECD) countries are overweight or obese. Although the overweight and obesity rates are much lower in Japan and Korea, the rates even in these countries are increasing. The prevalence of obesity, which presents even greater health risks than being overweight, varies approximately six-fold across OECD countries, from a low of 5% in Japan and Korea, to over 32% in Mexico and the United States [18]. Obesity is known to be associated with various medical and psychological comorbidities, increases cardiovascular and all-cause mortality. Although dietary and lifestyle modification are the mainstay of obesity management, it is a huge challenge for the majority of patients to permanently maintain their eating behaviors. Sustained weight loss after lifestyle modification and pharmacotherapy is achieved in less than 5% of cases [19,20]. Bariatric surgery is more effective and durable in inducing weight loss and decreasing obesity-related morbidities and mortality. However, early and late complications remain as high as 30%, and less than 1% of eligible patients undergo surgery [21]. Consequently, there has been a need for alternative weight loss therapies that are less invasive and less risky than bariatric surgery and more effective and durable than lifestyle interventions. Recently, endoscopic bariatric therapy (EBT) has been developed to fill the gap between medical and surgical therapy. Two main endoscopic weight loss modalities are restrictive and malabsorptive [22]. The main objective of restrictive procedures is to reduce the stomach volume by space-occupying devices and/or by suturing or stapling techniques that change gastric anatomy while malabsorptive procedures tend to prevent food contact with the duodenum and proximal jejunum. Additionally, EBTs can mimic some of the anatomic alterations created by bariatric surgery by selectively targeting the stomach or the small intestines [23]. In this review, endoluminal devices are separately described by their target organ: gastric and small-bowel endoscopic devices.
Gastric intervention and devices
OverStitch for endoscopic sleeve gastroplasty
The Apollo OverStitch (Apollo Endosurgery, Austin, TX, USA) is an endoscopic suturing device that applies full-thickness sutures in a variety of patterns. This device attaches proximally and distally to a dual channel flexible endoscope allowing for endoluminal suturing in multiple applications. The handle of device, mounted to the endoscope control handle, actuates the needle driver attached at the distal end. An anchor exchange catheter is placed in one scope channel to manage the passing of the suture, while the secondary channel can be utilized to operate the tissue helix for atraumatic tissue manipulation. Once the suturing pattern is completed, a cinching tool is deployed to provide knotless fixation. This suturing device enable running and interrupted stitches. In 2012, Thompson and Hawes reported the first human case of endoscopic sleeve gastrectomy (ESG) [24]. Possible mechanisms of action of EGS are decreased ghrelin without significant changes in peptide tyrosine tyrosine (PYY) or glucagon-like peptide 1 (GLP-1) levels, delayed gastric emptying and increased satiation, similar with laparoscopic sleeve gastroplasty [25]. This procedure was later modified to include medial interrupted reinforcing sutures based on the work of Abu Dayyeh et al., which reported a series of 4 patients who underwent a version of ESG using 2 rows of interrupted stitches [26]. Sharaiha et al. performed ESG on 10 patients [27]. Mean excess weight loss (EWL) were 18% after 1 month, 26% after 3 months, and 30% after 6 months [27]. Subsequently, other investigators have reported similar results [28,29]. Recently another multicenter trial reported 48.2%┬▒9.9% of EWL at 12 months in 20 patients without serious AEs [30].
Intragastric balloon
So far, 3 intragastric balloons (IGBs) were approved by the Food and Drug Administration (FDA) for the management of obesity. The Orbera IGB (Apollo Endosurgery, Austin, TX, USA), the ReShape Duo (ReShape Medical, San Clemente, CA, USA); and the Obalon IGB (Obalon Therapeutics Inc., Carlsbad, CA, USA). All 3 are approved to be used for 6 months (Fig. 3, Table 1). It is assumed that IGB facilitate weight loss by reducing the stomachŌĆÖs potential volume and inducing early satiety. In this way, total caloric intake for the day may be reduced. Action mechanism of IGB is not fully understood yet. Additional proposed mechanisms include changes in gastric emptying and hormonal changes. Gomez et al. reported that gastric emptying in subjects with IGB is delayed but returns to normal after IGB removal and greater changes in increased gastric retention were associated with greater percentage of total body weight loss (%TBWL) [31]. Other proposed mechanisms include changes in hormones. Mion et al. reported that gastric emptying rates and plasma ghrelin levels were decreased in the presence of IGB and weight loss induced by the IGB was related to ghrelin variations, but not to gastric emptying [32]. Ghrelin inhibition may explain part of the effect of the balloon on satiety [32]. However, there are conflicting reports of observed hormonal changes in other studies and therefore, the mechanism of action appears to be multifactorial. The most common AEs include nausea, vomiting, and decreased oral intake. Many of these symptoms can be managed conservatively without the need for early balloon removal. In a large retrospective study of 2,515 patients with IGB, overall complication rate was 70/2,515 (2.8%) with 5 perforations, 4 of whom had undergone previous gastric surgery, and 2 deaths, 32 esophagitis and 5 gastric ulcers [33]. A randomized, controlled trial observed only minor AE including belching and heartburn without any serious AEs [34].
Transpyloric shuttle
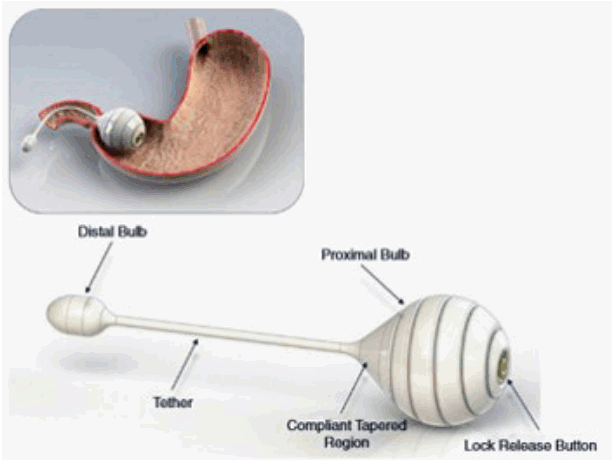
Transpyloric shuttle (TPS; BAROnova, Goleta, CA, USA) is a nonsurgical device that is endoscopically delivered to and removed from the stomach. The device consists of a large spherical bulb connected to a smaller cylindrical bulb by a flexible tether (Fig. 4). The larger bulb is designed to prevent migration from the stomach, while the smaller bulb passes freely into the duodenum to position the TPS across the pylorus. Transpyloric positioning may delay gastric emptying, reducing caloric intake and enabling weight loss. The TPS appears to have several mechanisms of action that promote weight loss. The large bulb, although the size is not as large as the IGBs, may partially reduce functional gastric volume. During antral contractions, the large bulb repeatedly engages the pylorus, causing intermittent obstruction. This action delays gastric emptying, prolongs gastric accommodation, and increases satiety. It is possible that the distal bulb is interacting with duodenal mucosa and incretin signaling, although this remains to be elucidated [35]. The TPS device is designed for temporary placement and does not fundamentally alter the gastrointestinal (GI) anatomy. One clinical study reported percentage of EWL (%EWL) of 25.1%, and percentage of total weight loss (%TWL) of 8.9% in 3 months and %EWL of 41.0%, %TWL of 14.5% in 6month without complications [36]. A 12 months multi-center prospective study (ENDObesity II Study) completed enrollment of 270 patients in 9 sites in the United States in December of 2016.
Small intestinal intervention and devices
The proximal small bowel plays an important role in glucose homeostasis. Also known as the incretin effect, oral glucose intake leads to amplification of insulin secretion compared with intravenous infusion. This effect is understood to be owing to gut hormones, such as incretins, peptide YY and oxyntomodulin [37-39]. In addition to their effect on glucose homeostasis, these gut hormones also affect satiety and GI motility. Therefore, small-bowel interventions may contribute to weight loss as well as diabetes improvement [40].
Duodenal jejunal bypass sleeve
Duodenal-jejunal bypass sleeve (DJBS; GI Dynamics, Lexington, MA, USA) is a reversible procedure developed to treat obesity and type 2 diabetes (Fig. 5) [41]. DJBS consists of a metallic anchor (Nitinol) that attaches the implant to the duodenum bulb and a 60 cm long GI liner that extends from duodenum to the proximal jejunum. It essentially mimics the intestinal bypass part of the Roux-en-Y surgery. DJBS with flow restrictor is a modification of DJBS which includes a 4 mm restrictor orifice distal to the anchor to slow gastric emptying in addition to the DJBS-mediated effects. Devices are temporary implants and can be removed after predetermined time interval [42]. The DJBS implantation procedure is performed using an endoscope and fluoroscopy [43-48]. The efficacy and safety, investigated by several studies showed %EWL of 30%ŌĆō47% at 52 weeks [49,50]. This device also appears to have efficacy in improving glycemic control, insulin resistance, and lipid profile [42]. However, a recent meta-analysis reported that an average of 0.9% change in HbA1c was observed and failed to show statistical significance [46]. Therefore, more researches are necessary to find out if DJBS can be an alternative therapy for management of type 2 diabetes and morbid obesity.
Duodenal mucosal resurfacing
The Revita duodenal mucosal resurfacing (DMR) procedure (Fractyl Laboratories Inc., Cambridge, MA, USA) involves the use of RF ablation following saline lift to induce mucosal remodeling. This may result in changes in enteroendocrine cells improving diabetic control [51]. The result of a single center, single-arm, open-label, nonrandomized study of DMR in type 2 diabetes to evaluate six-month safety and efficacy has recently been published [52]. HbA1c was reduced by 1.2% at 6 months and longer segment ablation showed more reduction of HbA1c of 2.5%, compared to 0.7% in short segment ablation group at 6 months. In 3 patients, duodenal stenosis occurred and treated successfully by balloon dilation. Long-term safety, efficacy, and durability and possible mechanisms of action require further investigation.
CONCLUSIONS
Thanks to the recent development of novel endoluminal devices, there have been remarkable progress in endoscopic management in GERD and obesity, although PPIs in GERD and surgery in Obesity remain the mainstay of the treatment. Endoscopic management may bridge the gap between medication and surgery. In addition, because these conditions are chronic, combining devices with different action mechanism or combing drug-device may allow better management of these diseases in the long term. However, more studies with long-term follow-up and randomized comparisons are required to establish its precise role and to understand the mechanisms of actions of each devices and methods.