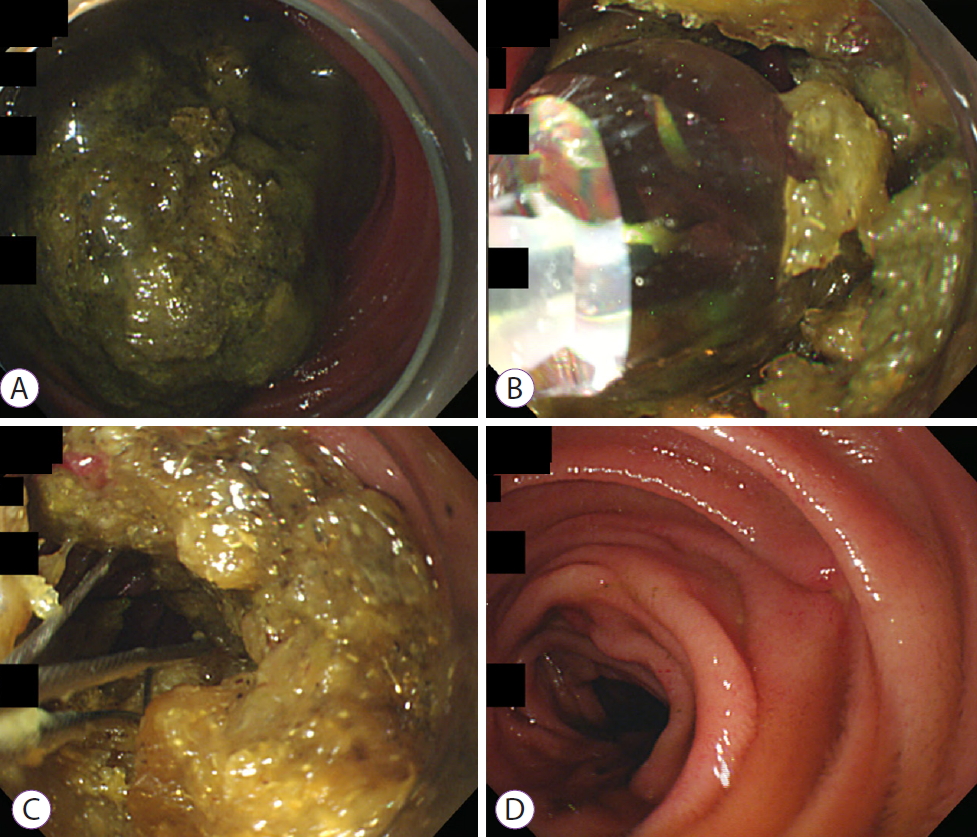
A 65-year-old woman presented to the emergency department with abdominal pain, distension, and vomiting that had persisted for five days. She had undergone subtotal gastrectomy for gastric cancer two years earlier. She did not take any medication. Physical examination revealed epigastric tenderness and increased bowel sound. A computed tomography scan revealed a 2.8├Ś3.8 cm mass with mottled gas pattern in the mid-jejunum along with marked dilatation of the stomach and proximal jejunum (Fig. 1). We performed peroral single-balloon enteroscopy (SIF-260; Olympus Co., Tokyo, Japan), which showed a yellowish-green phytobezoar occupying the entire lumen of the mid-jejunum (Fig. 2A). Our initial attempt to fragment the phytobezoar using forceps and snares was unsuccessful due to the hardness of the phytobezoar. To soften the phytobezoar wall, we administered 500 mL of Coca-Cola. The next day, a CRETM wire-guided balloon dilatation catheter (controlled radial expansion; Boston Scientific Co., Natick, MA, USA) was introduced into the softened phytobezoar. A guidewire with 0.025 inch in diameter was passed through the center of the phytobezoar and a 10ŌĆō12 mm balloon catheter was placed. We then inflated the balloon to 12 mm to fragment the bezoar (Fig. 2B). Additionally, we used a Dormia basket (Cook Medical, Bloomington, IN, USA) to gradually fragment the phytobezoars into even smaller pieces (Fig. 2C). The total procedure time was 50 minutes and no complications were noted. An enteroscope inserted into the small intestine cannot be removed perorally with the cap attached and all procedures must be completed in the scope-inserted state. Therefore, we could not retrieve the bezoar fragments from the jejunum. After endoscopic treatment, a low-volume polyethylene glycol (PEG) (2 L) plus ascorbic acid solution (Coolprep┬«; TaeJoon Pharmaceuticals, Seoul, Korea) was administered, and the patientŌĆÖs symptoms disappeared. A computed tomography scan three days later showed no obstruction or residual phytobezoar. The patient was discharged after bezoar resolution (Fig. 2D and Supplementary Videos 1).
Bezoars are defined as hard masses in the gastrointestinal (GI) tract, which are composed of indigestible organic material. Based on their composition, bezoars are classified as phytobezoars (plant material), diospyrobezoars (unripened persimmons), pharmacobezoars (medication), lactobezoars (inspissated milk), and trichobezoars (hair) [1]. They are most commonly found in the stomach, although they can occur in any segment of the GI tract, including the esophagus, small bowel, and colon; however, jejunal localization is very rare. Bezoars may occur in individuals with previous gastric surgery including vagotomy or pyloroplasty, intestinal dysfunction, neuropathy in diabetic patients, hypothyroidism, psychiatric or developmental disorders, and chronic antacid treatment [2]. Bezoar-induced small bowel obstruction in patients with previous gastrectomy is well known as a late complication, with an incidence rate of 5%ŌĆō12% [3]. Small bowel bezoars manifesting obstruction, ischemia, or perforation should be managed surgically if other modalities are unsuccessful [4]. However, surgical treatments, including manually fragmenting the bezoar and expelling it towards the cecum, enterotomy, and segmental bowel resection, are often associated with higher morbidity and mortality compared to endoscopic management. There have been few descriptions of non-surgical treatment for small bowel bezoars. We believe only four cases of bezoar-induced small bowel obstruction have been treated successfully by balloon-assisted enteroscopy [5-8]. To ensure success in our case, we softened the phytobezoar by injecting it with carbonated liquid (Coca-Cola) using an injection needle. Next, a CRETM wire-guided balloon dilatation catheter was inserted into the center of the phytobezoar to crush it; further, it was fragmented into smaller pieces using a Dormia basket. Additionally, to prevent re-obstruction, the fragmented phytobezoar was released into the feces using a PEG solution. Our experience in removing a large bezoar stuck at the mid-jejunum suggests that balloon-assisted enteroscopy, which is safe, effective, and minimally invasive, is a suitable initial approach and an ideal substitute for surgery.