INTRODUCTION
Cholecystectomy is the gold standard treatment for gallbladder stone disease.1 However, 10%ŌĆō30% of patients complain of upper abdominal pain, dyspepsia, or jaundice after a cholecystectomyŌĆöthis is referred to as postcholecystectomy syndrome (PCS).2 There are several causes of PCS such as cystic duct stump stone, remnant gallbladder stone, common bile duct (CBD) stone, and biliary stricture.3
Cystic duct stump stones are a troublesome cause of PCS. An open completion cholecystectomy or second laparoscopic cholecystectomy is often preferred to treat cystic duct stump stones.4 However, repeated surgery can cause complications such as postoperative bleeding, biliary injury, and wound infection.5 Furthermore, some patients who have high risk factors for surgery are very reluctant to undergo a second surgery. Endoscopic retrograde cholangiopancreatography (ERCP) is often used as an alternative to surgical treatment to remove cystic duct stump stones. However, reaching the tortuous cystic duct and removal of the impacted stone is technically very challenging; thus, the success rate is not satisfactory.3 The single-operator cholangioscopy (SOC) is a new type of peroral cholangioscopy (POCS): it uses a device that allows direct observation of the bile duct and it is often used for the removal of challenging bile duct stones, as well as for the accurate diagnosis of bile duct diseases.6
We report two cases of successful removal of the cystic duct stump stone using a SOC-guided electrohydraulic lithotripsy (EHL).
CASE REPORTS
Case 1
A 28-year-old male patient visited because of right upper abdominal pain that had occurred the previous day. He had no specific medical or surgical history. The initial laboratory data were within the normal range. Abdominopelvic computed tomography (CT) revealed distension of the gallbladder with a stone and wall thickening. The patient underwent a laparoscopic cholecystectomy and recovered uneventfully.
Two months later, he visited the hospital again with epigastric pain. The laboratory data were as follows: white blood cell (WBC), 17,020/mm3; aspartate aminotransferase (AST), 92 IU/L; alanine aminotransferase (ALT), 229 IU/L; total bilirubin, 3.16 mg/dL; alkaline phosphatase (ALP), 122 IU/L; and C-reactive protein (CRP), 1.96 mg/dL.
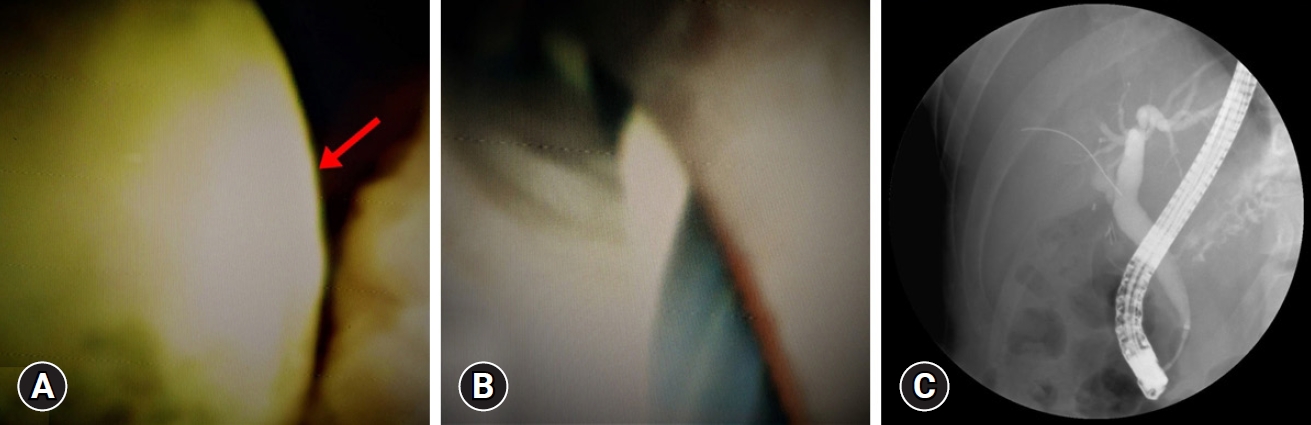
Magnetic resonance cholangiopancreatography (MRCP) showed that an 8-mm sized stone impacted the remnant cystic duct, compressed the proximal CBD, and dilated the remnant cystic duct stump and proximal extrahepatic duct (Fig. 1A). An ERCP was attempted, but the stone was firmly stuck in the cystic duct stump and did not move with basket or balloon sweeping (Fig. 1B). An endoscopic retrograde biliary drainage stent was inserted, and the patientŌĆÖs symptoms and blood tests improved.
After two months, an ERCP was performed again, but the stone removal failed. We recommended surgical treatment, but the patient refused for personal reasons. Therefore, SOC-guided EHL was performed to remove the cystic duct stump stones.
First, SOC using the SpyGlassDS system (Boston Scientific Corp.) was introduced into the biliary trees, and the stone was observed. Under direct vision, the stone was fragmented by EHL (Lithotron EL27; Walz Elektronik GmbH) with an initial intensity of 250 mJ and pulse frequency of 60 Hz, which were escalated (as needed) to achieve stone fragmentation. The fragmented stone was removed using a basket and a balloon (Fig. 2A, B).
The patientŌĆÖs symptoms improved after the stone removal with SOC-guided EHL. Finally, the ERCP showed no evidence of cystic duct stump stones (Fig. 2C).
Case 2
A 38-year-old female patient visited the hospital with epigastric pain and vomiting persisting since the last five days. Her medical history indicated that she had been hospitalized 9 months before for acute cholecystitis with a resulting laparoscopic cholecystectomy. Apart from that, she had no specific medical history.
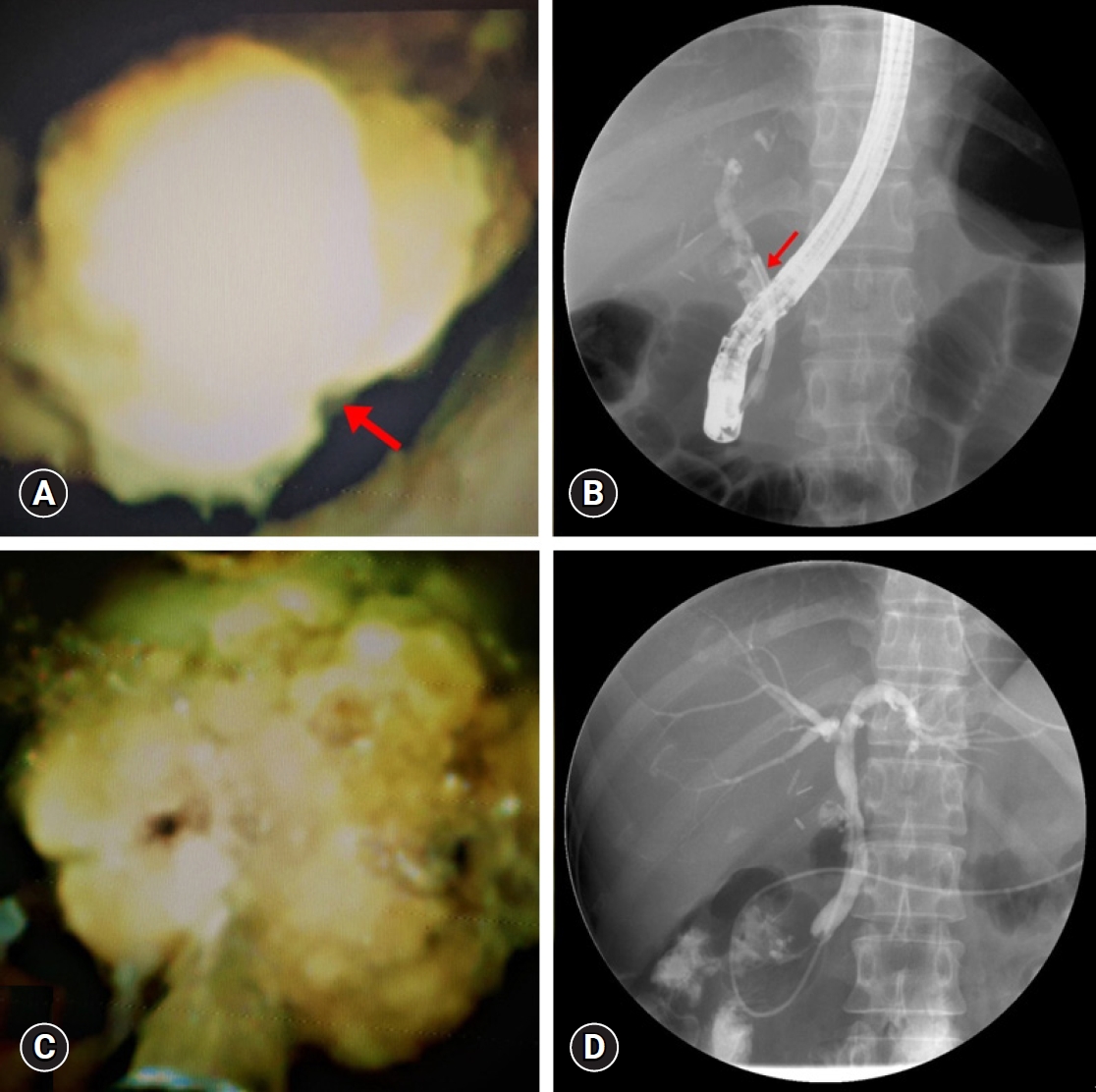
Blood test results were as follows: WBC, 9,860/mm3; AST, 106 IU/L; ALT, 316 IU/L; total bilirubin, 2.58 mg/dL; CRP, 10.4 mg/dL; and ALP, 317 IU/L. CT showed dilatation of the remnant cystic duct and CBD (Fig. 3A). An impaction of a large stone in the dilated cystic duct was observed using endoscopic ultrasonography (EUS).
We attempted an ERCP for the stone removal. However, the stone was firmly embedded in the cystic duct stump and could not be removed (Fig. 3B). Endoscopic nasobiliary drainage was inserted for drainage and decompression of the CBD. As the patient had a negative opinion about repeated surgery, SOC-guided EHL was attempted. After direct visualization of the cystic duct stone under the SOC, the targeted stone was fragmented using EHL (Fig. 4AŌĆōC). Follow-up ERCP confirmed that the stone was not visible (Fig. 4D).
DISCUSSION
PCS is described as the presence of complex symptoms such as upper abdominal pain, indigestion, and jaundice that continue after cholecystectomy. Other symptoms include vomiting, pancreatitis, and cholangitis.5 In general, women tend to have a higher incidence of PCS than men, with a male-to-female ratio of 1:1.45.7
Remnant gallbladder/cystic duct stump stones are uncommon causes of PCS. Its incidence is less than 2.5%ŌĆō16% among patients who undergo a cholecystectomy.8,9 The presence of residual cystic duct stump stones after a cholecystectomy may depend on the degree of gallbladder resection. Palanivelu et al.4 reported that the incidence of cystic duct stump stone after a laparoscopic subtotal cholecystectomy was 4.19% and 0.02% after a laparoscopic total cholecystectomy. A laparoscopic subtotal cholecystectomy is a method often used in patients with cirrhosis, or as an emergency surgery for acute cholecystitis. This is because the gallbladder, which is difficult to remove, can be resected without an incision of the Calot triangleŌĆöthereby reducing damage to the bile duct.1 The other causes are known to be poor visibility of the gallbladder fossa during surgery (due to adhesion), recurrent inflammation, or confounding gallbladder morphology (such as a long cystic duct).3
Abdominal ultrasound, CT, MRCP, ERCP, and EUS are all effective in diagnosing cystic duct stump stones1ŌĆöof which MRCP is the most accurate diagnostic method, which can detect cystic duct stump stones with an accuracy of 94%ŌĆō100%.1,10 MRCP is noninvasive and safe, providing clear anatomical and pathological images of the biliary tree.1 An EUS can be helpful when the abdominal ultrasound is negative, but that there is a strong suspicion of the presence of a cystic duct stump stone.11
The treatment of a cystic duct stump stone involves completion cholecystectomy, which can be performed either by laparoscopy or open cholecystectomy.5 Previously, open completion cholecystectomy was considered safer than a laparoscopy because it can avoid damage to the duodenum or colon when adhesions are severe, the cystic duct is embedded, and can also avoid damaging the bile duct.1,12 However, it is now accepted that laparoscopic access is also safe.3,5,13 One study reported on 40 patients who underwent laparoscopic completion cholecystectomy. Two of these cases were converted to open surgery due to adhesions, and only one case had a CBD injury. There were no cases of mortality.10 Nevertheless, surgery is an invasive method, and there is a risk of complications from general anesthesia to postoperative complications (such as bleeding and infection).
ERCP can be considered as an alternative surgery. However, removing cystic duct stump stones by ERCP is technically challenging and its success relies on various factors such as the size and number of stones, degree of stone impaction, diameter of the cystic duct, location of the stone in the duct, and angle between the cystic duct and CBD.3,10 There are few studies on the success rate of cystic duct stump stone removal through endoscopic treatment; England and Martin14 have reported that the success rate of endoscopic treatment was not as high as 52%.
Since the 1970s, POCS has been used to diagnose and treat various biliary diseases. It has also been used during lithotripsy to treat choledocholithiasis.15 A single-operator fiberoptic cholangioscope system, the SpyGlass Direct Visualization System, has been available since 2005. With the second-generation SpyGlass DS System, the quality and stability of images were improved.16 The best advantage of SOC is that it can provide direct visualization of all bile ducts and thus is used to treat difficult bile duct stones, as well as diagnose bile duct diseases under direct vision.
The effectiveness and stability of SOC in the treatment of difficult bile duct stones have already been demonstrated in several studies. Treatment of bile duct stones using SOC-guided EHL or laser lithotripsy showed a success rate of 80%ŌĆō98%.17 Although few reports exist in the literature, it is thought that the success rate of cystic duct stone removal using SOC is almost similar to that of bile duct stone removal. Therefore, it can be inferred that the success rate is higher than that of ERCP. Additionally, SOC with EHL is less invasive than surgery and complications are similar to those of ERCP.18
In our experience, a stepwise approach is recommended for the treatment of cystic duct stump stones persisting after cholecystectomy. ERCP would be the first procedure applicable. If it fails, the SOC with EHL can be used as an alternative. Surgery can be considered as the last step as a rescue method.
In conclusion, we report two cases in which the cystic duct stump stones, which were difficult to remove with an ERCP, were successfully removed with EHL via SOC using the SpyGlass DS system.