See commentary "There is no royal road: a shortcut for endoscopic submucosal dissection training" in Volume 56 on page 590 AbstractBackground/AimsWe developed a new endoscopic submucosal dissection (ESD) simulator and evaluated its efficacy and realism for use training endoscopists.
MethodsAn ESD simulator was constructed using polyvinyl alcohol hydrogel sheets and compared to a previous ESD simulator. Between March 1, 2020, and December 30, 2021, eight expert endoscopists from three different centers analyzed the procedure-related factors of the simulator. Five trainees performed gastric ESD exercises under the guidance of these experts.
ResultsAlthough the two ESD simulators provided overall favorable outcomes in terms of ESD-related factors, the new simulator had several benefits, including better marking of the target lesionтs limits (p<0.001) and overall handling (p<0.001). Trainees tested the usefulness of the new ESD simulator. The complete resection rate improved after 3 ESD training sessions (9 procedures), and the perforation rate decreased after 4 sessions (12 procedures).
INTRODUCTIONEndoscopic submucosal dissection (ESD) is a procedure used to treat early gastric cancer and is currently widely used for the treatment of gastrointestinal diseases, including early gastric cancer, esophageal cancer, and colon cancer.1-5 ESD has a lower medical cost, complication rate, and recovery time than surgery. However, a great deal of experience is required to acquire a high skill level and the associated risk of procedure-related complications is high. The complications and prognosis of patients depend on the expertise and precision of the operator.6,7
ESD was developed in Japan. Most of the training process is based on the тMaster-Apprentice process,т in which trainees receive one-on-one, step-by-step training under the guidance of an expert. Nonetheless, this process has a disadvantage in that it is only possible in regions where ESD is actively implemented.
Currently, several tools including textbooks, online video media, simulators, and hands-on sessions are used for self-ESD training outside Japan. These tools are helpful for learning about ESD procedures, although they have limitations. For example, aspects such as delicate endoscopic handling, injection, circumferential cutting, submucosal dissection, and handling of adverse events, such as bleeding and perforations, are more difficult to learn using these tools.8,9
In the past, animal models, such as ex vivo and in vivo porcine models, were commonly used to improve endoscopic handling; however, these methods also have several limitations.10,11 First, the preparation of animal models is expensive. Second, ESD training is only possible in animal operating rooms. Third, pigs have a thick stomach wall that contains a high volume of oil compared to that of humans; this makes it difficult for beginners to perform ESD. Fourth, additional training is impossible if perforation occurs while performing ESD on a live pig. Fifth, ethical concerns and restrictions regarding reusability are inherent to this method. To overcome these limitations, an ESD simulator using artificial tissue was introduced, although lifting the submucosal layer is impossible with this method.12
Recently, a new artificial ESD simulator, Endogel (Sunarrow, Tokyo, Japan), was developed for ESD/peroral endoscopic myotomy training.10,13 Endogel is a composite plate laminated with three types of polyvinyl alcohol hydrogel (PVA-H) sheets. Different types of PVA-H sheets with different elasticities can be laminated together to mimic the mucosa and submucosa; these can then be used in simulated procedures, such as mucosal incision, submucosal dissection, and muscle layer myotomy.13 There are no restrictions on where ESD can be administered. However, Endogel does have some limitations. First, it is quite expensive and is unavailable in some countries. Second, because the target lesion canтt be adjusted, the trainee canтt practice gastric ESD with the lesions in various locations. In this study, a new ESD simulator was developed and evaluated for its use by beginners for achieving a high level of technical experience before performing the procedure in patients.
METHODSParticipantsThirteen endoscopists (eight experts and five ESD trainees) participated in this evaluation of the ESD simulator from March 1, 2020 to December 30, 2021, at SMG-SNU Boramae Medical Center, Seoul National University Hospital, and Asan Medical Center, Seoul, Korea. The expert members from the staff of the three hospitals had experience performing ESD in over 500 human cases and 10 live pig cases. The five ESD trainees were endoscopists with experience performing over 2,000 cases of esophagogastroduodenoscopy and 500 cases of colonoscopy. The new ESD simulator was developed at Asan Medical Center, although the final evaluation was performed at SMG-SNU Boramae Medical Center to avoid subjectivity of the evaluation.
New gastric ESD simulatorThe new PVA-H-based ESD simulator was developed by an experienced endoscopist at the Asan Medical Center. This new simulator is composed of three units: the esophagus unit for endoscopic insertion, the gastric wall unit for injection and cutting, and the electric unit for radiofrequency current conduction and return function (Fig. 1). The esophagus unit is produced using stereolithography three-dimensional printing (OMG SLA 660 3D printer; Xiamen Zhisen Electro. Equip.) and a silicone molding technique (EchoFlex 0030; Smooth-On Inc.).14 The gastric wall unit is produced using a three-layered PVA-H (PVA 98т98.8% hydrolyzed, MW 146,000т186,000; Thermo Fisher Scientific Inc.) sheet. All materials used in the gastric wall units were edible grade or harmless to the human body. The gastric wall unit was 17У12У1.7 cm in size and composed of a three-layered PVA-H sheet. The first, second, and third layers were the mucosal, submucosal, and proper muscle layers, respectively. The PVA-H layers were polymerized by one to two freezeтthaw cycles. The final properties of the materials and thickness of each layer were optimized based on the thickness of the mucosal layer and incision of the submucosal layer. The electric unit had dual electrodes (KODE plate; KODE Medical Ind.) connected to the gastric wall unit that conducted the electric current (Fig. 1).
Outcome measuresTwo ESD simulators, an existing simulator (Endogel) and a new simulator (Asan ESD simulator; Asan Medical Center, Seoul, Korea), were evaluated for their performance by experts (Figs. 1, 2). The primary outcome was suitability for ESD training, which was measured by an expert group comprising staff from three different hospitals. After using the ESD simulator, the expert group evaluated it with a score table using a 7-point Likert scale (Table 1). The highest score reflected greater realism compared to the human gastric ESD. For example, a 7-point Likert scale for agreement will include as the following options: strongly disagree, disagree, somewhat disagree, either agree or disagree, somewhat agree, agree, and strongly disagree (1=strongly disagree; 2=disagree; 3=somewhat disagree; 4=either agree or disagree; 5=somewhat agree; 6=agree; 7=strongly agree). The score table covered the following topics: (1) ESD of the target lesion, (2) limitations, (3) complications, and (4) mechanical and electrical performance (Table 1). тMarkingт means circumscribe the limits of the target lesion using a dual knife (KD-655Q; Olympus). тSubmucosal injectionт refers to the injection of fluid into the submucosal layer around a lesion to separate it from the muscle layer. тMucosal incisionт means cutting the mucosa surrounding the lesion using a dual knife and an IT knife (KD-611L; Olympus) to obtain a circumferential incision with submucosal exposure. тSubmucosal dissectionт refers to cutting of the submucosal layer. тComplete resectionт means the resection of target lesion without tearing. Piecemeal resection does not include тcomplete resectionт. тVisibility after submucosal injectionт refers to the submucosal layer under the dissected mucosal layer. тCurling of the dissected lesionт refers to the curled mucosal lesion after submucosal dissection. тPerforation occurred in ESDт indicates perforation similar to that which occurs during ESD. тSufficient size for ESD trainingт means the test area for ESD training; the larger the size of the PVA-H, the greater the opportunities for gastric ESD being implemented by trainees. тConnectivity of the electrosurgical unit (ESU)т means the electric current from the ESU to the target area. тRealism of wall layerт refers to the suitability of the construction of the simulatorтs layers. The names of each layer are shown in Fig 1. A-3. Both simulators consisted of four layers; cutting of the third layer and exposure of the fourth layer (the serosa layer) was regarded as a perforation. Hence, when the sky-blue sponge was visible, it is considered a perforation.
The secondary outcomes were the learning curves when using the new ESD simulator, which were measured by the trainee group in the following aspects: (1) complete resection and (2) perforation, where тcomplete resectionт meant removal of the target lesion completely without tearing, and тperforationт meant the exposed muscle layer. Each trainee attempted ESD three times per session, for a total of five sessions. The results of three successful trails per session were recorded for each trainee. The total number of complete resections and perforations per session was recorded.
Details of the device settingWe used a standard single-channel endoscope (GIF-H290; Olympus), IT knife 2, electrosurgical unit (ERBE VIO 300D; Erbe), dual knife, soft transparent hood (D-201-13404; Olympus), and submucosal injection with normal saline and indigo carmine. ESD was performed by attaching a cap (Olympus) to the end of the endoscope.
The PVA-H was refrigerated with plastic wrap before use, as it is prone to dehydration and shrinkage in open air. The target lesions were 2-cm circular lesions, and a maximum of nine lesions could be made on the PVA-H sheet. The ESU settings were as follows: monopolar, Endocut Q (max 770 Vp) with effect 1, duration 3 (10 ms), and interval 3 (720 ms).
ESD procedureESD involved the following steps: marking, injecting fluid, cutting the surrounding mucosa, injecting additional fluid, and dissecting the submucosal layer. A dual knife was used for marking the limits of the lesion, approximately 5 mm from the lesion itself. An injection needle (NeedleMaster; Olympus) was used to inject fluid to separate the target lesion from the muscle layer. An IT knife 2 and a dual knife were used for circumferential incision of the mucosal lesion and submucosal dissection.
ESD requires an in-depth understanding of endoscopic evaluation of lesions and high-level endoscopic skills. In this study, experts provided training for the operation, precautions related to the procedure, and demonstrated the correct usage of the ESD simulator before trainees used the equipment and procedure and gave feedback to the trainees both during and after every session. First, ESD trainees were exposed to ESD-related books and video media. While observing the procedures performed by experts, they were educated on precautions and equipment usage. The ESD simulator practice was always followed with feedback from the expert relating to problems during the procedure. Overall, trainees were educated on the theory for one month, while the procedure was observed for three months; an additional month of training was required to complete five sessions. Three experts served as the primary educators.
Statistical analysesStatistical analyses were conducted using IBM SPSS software ver. 26.0 (IBM Corp.). Continuous variables were reported as medians with interquartile ranges. A t-test was conducted to compare continuous variables between the two groups, and two-sided p-values <0.05 were considered statistically significant.
RESULTSESD on target lesionThe expert group compared the suitability of the two (new and existing) ESD simulators (Fig. 2, Table 1). The both simulators provided favorable overall outcomes for procedure-related factors (Table 1). One expert performed ESD on three lesions per simulator (test sequence: new simulator then existing simulator). Compared to the existing simulator, the new simulator showed better scores for marking (6 [5т6] vs. 4 [3.8т4], p<0.001) and overall handling of the endoscope (5 [4.8т5] vs. 3 [2т3], p<0.001).
Nevertheless, the results regarding lifting of the submucosal layer (4.5 [4т5] vs. 4 [3.8т4], p=0.256) were not satisfactory. When the submucosal solution was excessively injected, the visibility was unsatisfactory (4 [4т5] vs. 4.5 [4т5], p=0.807) and the dissected lesion was not curled (3 [3т4] vs. 2.5 [2т3], p=0.005). As the PVA-H sheet does not curl, dissection was performed by lifting the dissected lesion with an endoscopic cap.
The mechanical performances of both simulators were also favorable. The sizes of the ESD sheets required by the simulators were suitable for practice (6 [5.8т6] vs. 5 [4т5], p=0.005). When the submucosal solution was not injected, it was possible to perform ESD on nine practice lesions; when the submucosal solution was injected, it was only possible to perform ESD on three lesions. There was no malfunction of the electrical device during any of the procedures. The three-layered PVA-H sheet was scored as having satisfactory quality for ESD practice (6 [5.8т6] vs. 5 [4.8т6], p=0.085). The ESU functioned well in terms of electrical connectivity (7 [7т7] vs. 7 [6.8т7], p=0.554).
The new simulator was able to access the lesion through the esophageal unit and change the location of the lesion. In cases of perforation, lesion detection and endoscopic clipping were also possible.
Learning curve of ESD trainingThe trainee group tested the new ESD simulator over five sessions. The submucosal injection procedure was minimized to reduce visual disturbance. To measure the learning curves, the successful complete resection and perforation rates were counted. The complete resection rate improved after 3 sessions (9 procedures), and the perforation rate decreased after 4 sessions (12 procedures) of ESD training (Fig. 3, Table 2).
DISCUSSIONWe developed a new ESD simulator that is compatible with any endoscopic equipment. The ESD experts in our study approved its suitability for training and its potential to improve patient safety. The traineesт ESD skill levels improved as the number of training sessions increased.
ESD is an effective treatment option for various gastrointestinal diseases. Nonetheless, a great deal of time and experience are required to minimize ESD-related complications, such as bleeding and perforation. Various ESD simulators have been introduced to provide ESD-related training. Live porcine models are the most commonly used, and have been shown to accelerate the learning curve for gastric ESD training.15 Nevertheless, there are many limitations with ESD training using porcine models. Recently, a PVA-H-based ESD simulator, Endogel, was introduced, and its demand has been increasing despite its limitations.13
The new PVA-H-based ESD simulator has the following merits. First, any conventional endoscopic equipment is fully compatible with it. Second, its esophageal unit is more effective for practicing gastric ESD. Third, because the target lesion can be adjusted, the trainee can practice gastric ESD with the lesions in various locations. Owing to the considerable width of the ESD sheet, the trainee can create multiple lesions and perform gastric ESD several times. Fourth, the gastric ESD process can be viewed directly as well as through a monitor, which can help improve the proficiency of the practitioner. Fifth, the process of mucosal lifting and cutting in the simulator closely resembled that in human gastric ESD. Sixth, the amount of foam generated from the PVA-H sheets does not interfere with the procedure. Seventh, there is no danger of electric circuit connections and shock problems related to operator safety for the trainee during ESD. Eighth, compared with Endogel, the new simulator is 50% cheaper and readily available in all countries. Ninth, compared to animal models and conventional simulators, the new gastric ESD simulator may be a favorable alternative due to its reasonable performance, greater availability, and lower price.
The PVA-H-based simulator has the following limitations. First, it can only simulate ESD with flat lesions. Second, upon excessive submucosal injection, the injected solution causes visual disturbance, making it difficult to dissect the incised lesion. Therefore, skipping submucosal injection is recommended. For ESDs involving submucosal injection, it is suitable for performing three ESDs. If submucosal injection is omitted, it becomes suitable for performing nine ESDs. Nine ESDs appeared to be appropriate for simple training purposes, but not for research use (Fig. 2D). In future multi-center studies, it would be beneficial to consider ESD for nine lesions to reduce costs. Third, because the PVA-H sheet contained moisture, it had to be sealed and refrigerated. Fourth, it was difficult to reuse the PVA-H sheets. Fifth, sufficient ventilation was required because of the fumes emitted by the dissection sheet. Sixth, as the PVA-H sheet is not curled like the gastric wall, a cap must be attached to the end of the endoscope during practice. Seventh, although ESD simulators can help beginners begin performing and become proficient with the procedure, their role is limited, as they cannot train beginners how to deal with complications such as bleeding and perforation, which can occur in actual clinical settings.
The results of the current study should be interpreted in light of some limitations. First, a selection bias could have been present because of the small number of participants. Second, it is difficult to practice ESD for lesions located on a curved surface using the ESD simulator, as the ESD sheet is only made with a flat surface. Third, there could be bias and subjectivity in the evaluation because the scoring system was constructed using questionnaires. However, various evaluation indices and expert evaluators from other centers were employed to compensate for these limitations. For future research, it would be beneficial to conduct a multi-center study.
In conclusions, the new ESD simulator has several advantages such as its improved realism and affordability. We believe that this new ESD simulator will help improve practitionersт skills and ultimately improve patient safety and prognosis.
NOTESFig.Т 1.The new endoscopic submucosal dissection (ESD) simulator is composed of three units: the esophagus, gastric wall, and electric units. (A-1) The esophagus unit aids endoscopic insertion. (A-2) The gastric wall unit is connected to an electric surgical unit. (A-3) The gastric wall unit is designed to have three layers of different types of polyvinyl alcohol hydrogel (PVA-H) sheets. (A-4) An electric surgical unit. (B) An existing ESD simulator is composed of three units. 
Fig.Т 2.Demonstration of the two endoscopic submucosal dissection (ESD) simulators. (A) The new simulator. (B) The existing simulator. (C) Demonstrations of ESD with the new simulator; a direct view from above the simulator. (C-1) Marking of the target lesion. (C-2) Submucosal injection. (C-3) Circumferential cutting. (C-4) Submucosal dissection. (D-1) ESD with submucosal injection. (D-2) ESD without submucosal injection. 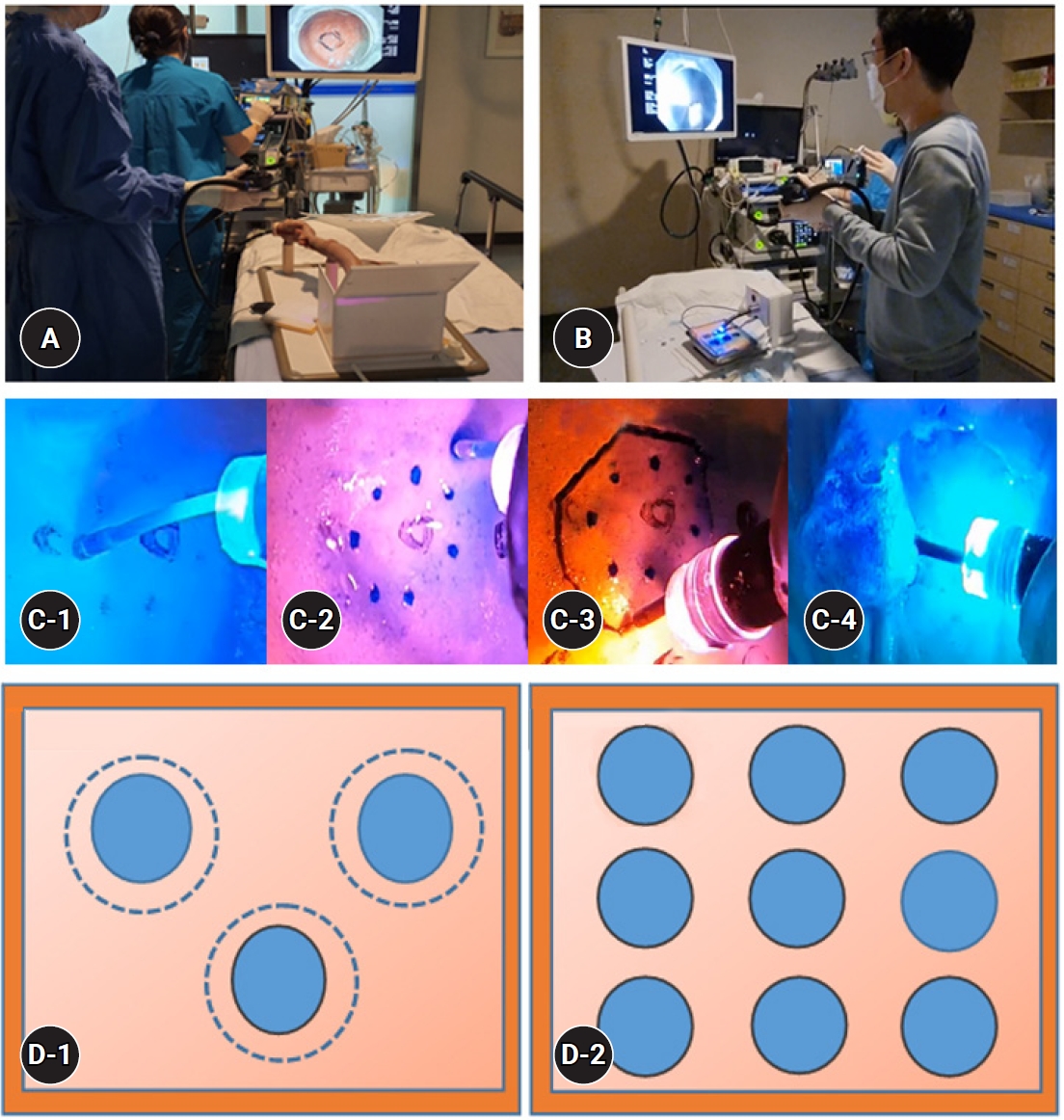
TableТ 1.Suitability of simulators for ESD training based on the 7-point Likert scalea)
TableТ 2.Learning curves for successful complete resection and perforation rates using the new ESD simulator, measured in the beginner group. REFERENCES1. Kang KJ, Kim KM, Min BH, et al. Endoscopic submucosal dissection of early gastric cancer. Gut Liver 2011;5:418т426.
2. Gotoda T, Yamamoto H, Soetikno RM. Endoscopic submucosal dissection of early gastric cancer. J Gastroenterol 2006;41:929т942.
3. Ohkura Y, Iizuka T, Kikuchi D, et al. Endoscopic submucosal dissection for early esophageal cancer associated with achalasia. Turk J Gastroenterol 2013;24:161т166.
4. Holmstrom AL, Aadam AA, Hungness ES. Submucosal endoscopy. Tech Gastrointest Endosc 2018;20:211т217.
5. Pasricha PJ, Hawari R, Ahmed I, et al. Submucosal endoscopic esophageal myotomy: a novel experimental approach for the treatment of achalasia. Endoscopy 2007;39:761т764.
6. Odagiri H, Yasunaga H. Complications following endoscopic submucosal dissection for gastric, esophageal, and colorectal cancer: a review of studies based on nationwide large-scale databases. Ann Transl Med 2017;5:189.
7. Toyokawa T, Inaba T, Omote S, et al. Risk factors for perforation and delayed bleeding associated with endoscopic submucosal dissection for early gastric neoplasms: analysis of 1123 lesions. J Gastroenterol Hepatol 2012;27:907т912.
8. Lee EJ, Lee JB, Choi YS, et al. Clinical risk factors for perforation during endoscopic submucosal dissection (ESD) for large-sized, nonpedunculated colorectal tumors. Surg Endosc 2012;26:1587т1594.
9. Toyonaga T, Man-i M, Fujita T, et al. Retrospective study of technical aspects and complications of endoscopic submucosal dissection for laterally spreading tumors of the colorectum. Endoscopy 2010;42:714т722.
10. Mizuno K, Sato H, Hashimoto S, et al. A novel training model composed of nonbiological materials for endoscopic submucosal dissection. Gastrointest Endosc 2016;84:373т374.
11. Ohata K, Nonaka K, Misumi Y, et al. Usefulness of training using animal models for colorectal endoscopic submucosal dissection: is experience performing gastric ESD really needed? Endosc Int Open 2016;4:E333тE339.
12. Chen MJ, Wang HY, Chang CW, et al. A novel artificial tissue simulator for endoscopic submucosal resection training: a pilot study. BMC Gastroenterol 2016;16:112.
13. Sato H, Mizuno KI, Sato Y, et al. Development and use of a non-biomaterial model for hands-on training of endoscopic procedures. Ann Transl Med 2017;5:182.
14. Smooth-On Inc. Product brochure [Internet]. Macungie: Smooth-On Inc. [cited 2020 Dec 30]. Available from: https://www.smooth-on.com/products/ecoflex-00-30/.
|
|
|||||||||||||||||||||||||||||||||||||||||
